Non-Hodgkin lymphoma (also known as non-Hodgkin’s lymphoma, NHL, or sometimes just lymphoma) is a cancer that starts in cells called lymphocytes, which are part of the body’s immune system. Lymphocytes are in the lymph nodes and other lymphoid tissues (such as the spleen and bone marrow). These will be described in more detail further on.

Some other types of cancer – lung or colon cancers, for example – can spread to lymph tissue such as the lymph nodes. But cancers that start in these places and then spread to the lymph tissue are not lymphomas.
The main types of lymphomas are:
These different types of lymphomas behave, spread, and respond to treatment differently.
Doctors can usually tell the difference between them by looking at the cancer cells under a microscope. In some cases, sensitive lab tests may be needed to tell them apart.
Hodgkin disease is discussed in a separate American Cancer Society document. We also have other documents that focus on non-Hodgkin lymphoma in children and lymphoma of the skin.
Symptoms
Some common non-Hodgkin lymphoma symptoms include:
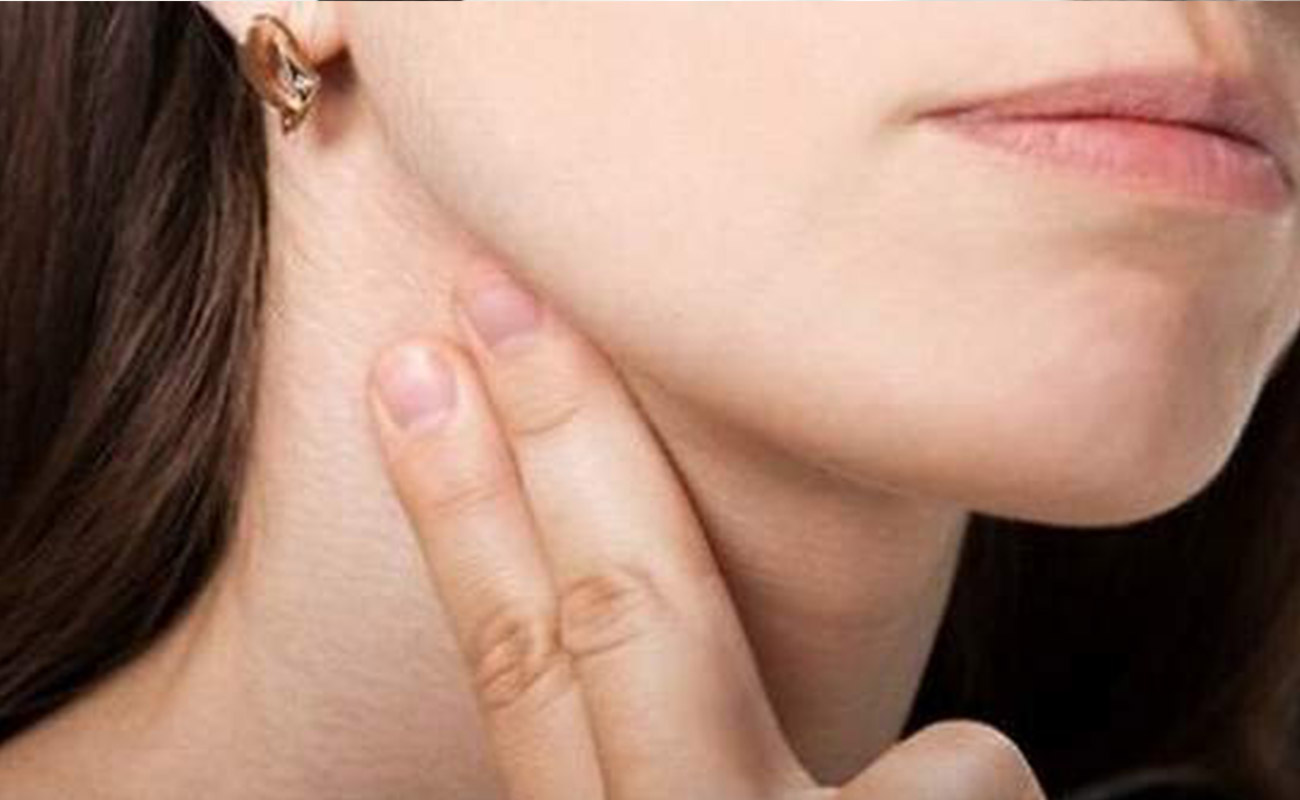
Swollen lymph nodes, a fever and night sweats may also be symptoms of the cold and flu. However, unlike the cold and flu, non-Hodgkin lymphoma symptoms typically do not go away. If you have symptoms that persist for more than two weeks, or symptoms that are recurring and becoming more intense, you should see your doctor.
Dramatic weight loss in a short amount of time, such as losing more than 10 percent of your normal weight in less than six months, is also a sign to seek medical attention. Sometimes, the only NHL symptom present is constant fatigue.
Causes
Doctors aren't sure what causes non-Hodgkin's lymphoma.
Non-Hodgkin's lymphoma occurs when your body produces too many abnormal lymphocytes — a type of white blood cell.
Normally, lymphocytes go through a predictable life cycle. Old lymphocytes die, and your body creates new ones to replace them. In non-Hodgkin's lymphoma, your lymphocytes don't die, but continue to grow and divide. This oversupply of lymphocytes crowds into your lymph nodes, causing them to swell.
Non-Hodgkin's lymphoma can begin in the:
Subtypes of non-Hodgkin's lymphoma that involve B cells include diffuse large B-cell lymphoma, follicular lymphoma, mantle cell lymphoma and Burkitt lymphoma.
Subtypes of non-Hodgkin's lymphoma that involve T cells include peripheral T-cell lymphoma and cutaneous T-cell lymphoma.
Whether your non-Hodgkin's lymphoma arises from your B cells or T cells helps to determine your treatment options.
Non-Hodgkin's lymphoma generally involves the presence of cancerous lymphocytes in your lymph nodes, but the disease can also spread to other parts of your lymphatic system. These include the lymphatic vessels, tonsils, adenoids, spleen, thymus and bone marrow. Occasionally, non-Hodgkin's lymphoma involves organs outside of your lymphatic system.
Diagnosis
Tests and procedures used to diagnose non-Hodgkin's lymphoma include:
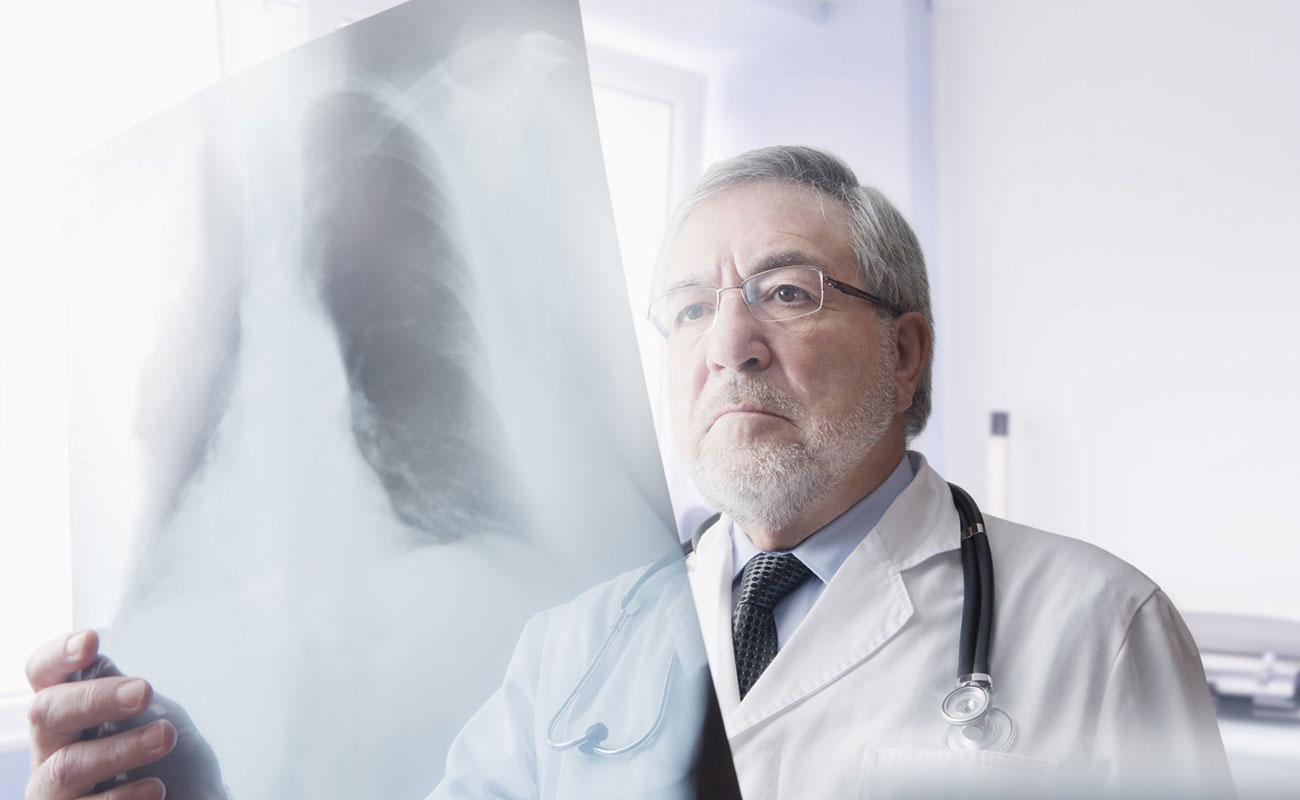
If the disease is low-grade (slow developing) and you're well, a period of "watchful waiting" is often recommended. This is because some people take many years to develop troublesome symptoms and starting treatment immediately is often felt to be unnecessary.
If watchful waiting is recommended, you'll be seen regularly for reviews and invited to come back at any stage if you feel your symptoms are getting worse.
Chemotherapy is a widely used treatment for non-Hodgkin lymphoma, which involves using medicine to kill cancer cells. It may be used on its own, combined with biological therapy and/or combined with radiotherapy (see below).
The medication can be given in a number of different ways, depending on the stage of your cancer.
If doctors think your cancer is curable, you'll normally receive chemotherapy through a drip directly into a vein (intravenous chemotherapy). If a cure is unlikely, you may only need to take chemotherapy tablets to help relieve your symptoms.
If there's a risk of the cancer spreading to your brain, you may have chemotherapy injections directly into the cerebrospinal fluid around your spine.
Chemotherapy is usually given over a period of a few months on an outpatient basis, which means you shouldn't have to stay in hospital overnight. However, there may be times when your symptoms or the side effects of treatment become particularly troublesome, and a longer hospital stay may be needed.
Chemotherapy can have several side effects, the most significant of which is potential damage to your bone marrow. This can interfere with the production of healthy blood cells and cause the following problems:
If you experience these problems, treatment may need to be delayed so you can produce more healthy blood cells. Growth factor medicines can also stimulate the production of blood cells.
Other possible side effects of chemotherapy include:
Most side effects should pass once your treatment has finished. Tell your care team if side effects become particularly troublesome, as there are treatments that can help.
Read more about the side effects of chemotherapy.
If non-Hodgkin lymphoma doesn't get better with initial treatment (known as "refractory" lymphoma), you may have a course of chemotherapy at a stronger dose.
However, this intensive chemotherapy destroys your bone marrow, leading to the problems mentioned above. You'll need a stem cell or bone marrow transplants to replace the damaged bone marrow.
Radiotherapy is most often used to treat early-stage non-Hodgkin lymphoma, where the cancer is only in one part of the body.
Treatment is normally given in short daily sessions, Monday to Friday, over several weeks. You should not have to stay in hospital between appointments.
Radiotherapy itself is painless, but it can have some significant side effects. These can vary, depending on which part of your body is being treated. For example, treatment to your throat can lead to a sore throat, while treatment to the head can lead to hair loss.
Other common side effects include:
Most side effects are temporary, but there's a risk of long-term problems, including infertility and permanently darkened skin in the treatment area.
Read more about:
For some types of non-Hodgkin lymphoma, you may have a type of medication called a monoclonal antibody.
These medications attach themselves to the surface of cancerous cells and stimulate the immune system to attack and kill the cells. They're often given in combination with chemotherapy to make the treatment more effective.
For some types of non-Hodgkin lymphoma, you may continue having monoclonal antibody treatment regularly for up to two years after initial treatment, in combination with chemotherapy. This can reduce the chances of the cancer coming back in the future.
One of the main monoclonal antibody medications used to treat non-Hodgkin lymphoma is called rituximab. This medication is administered directly into your vein over the course of a few hours.
Side effects of rituximab can include:
You may be given additional medication to prevent or lessen these side effects. Side effects should improve over time, as your body gets used to rituximab.
As rituximab has been so successful in treating non-Hodgkin lymphoma, scientists are working hard to make more monoclonal antibody treatments for lymphoma, and some of these are already at an advanced stage in clinical trials. You may be asked if you want to participate in one of these trials during your treatment.
Steroid medication is commonly used in combination with chemotherapy to treat non-Hodgkin lymphoma. This is because research has shown that using steroids makes the chemotherapy more effective.
The steroid medication is normally given as tablets, usually at the same time as your chemotherapy. A short course of steroids, lasting no more than a few months, is usually recommended, as this limits the number of side effects you could have.
Common side effects of short-term steroid use include:
On rare occasions, you may have to take steroids on a long-term basis. Side effects of long-term steroid use include weight gain and swelling in your hands, feet and eyelids.
The side effects of steroid medication usually start to improve once treatment finishes.
After your course of treatment ends, you may have a repeat scan to see how well the treatment has worked. Following this, you'll need regular follow-up appointments to monitor your recovery and check for any signs of the cancer returning (known as a "relapse").
These appointments will start off being every few weeks or months, but become less frequent over time.
Sources: cancer.org, cancercenter, mayoclinic.org, nhs.uk
Submit Comment