Vitrectomy is a surgical procedure undertaken by a specialist where the vitreous humor gel that fills the eye cavity is removed to provide better access to the retina. This allows for a variety of repairs, including the removal of scar tissue, laser repair of retinal detachments and treatment of macular holes. Once surgery is complete, saline, a gas bubble or silicone oil may be injected into the vitreous gel to help hold the retina in position.
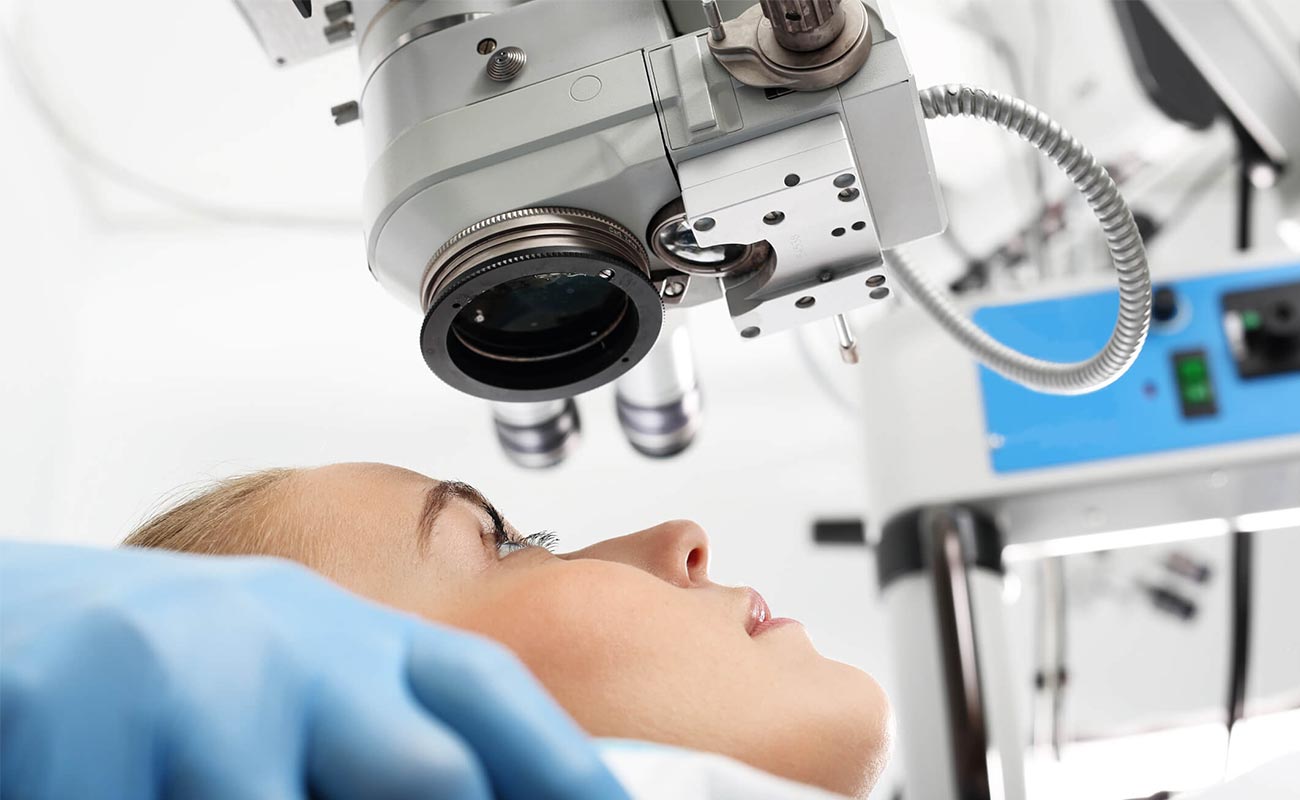
Trans pars plana vitrectomy (TPPV) is used to treat many retinal disorders such as:
Proliferative diabetic retinopathy (including vitreous hemorrhage)
Macular hole
Epiretinal membrane (macular pucker)
Complicated, tractional or recurrent retinal detachment
Intraocular infections (endophthalmitis)
Intraocular foreign body
Retained lens material or dislocated lens implants following cataract surgery
Giant retinal tears
Age related macular degeneration
Eye injuries
Uveitis
Long term support of the retina as is required in the repair of very complicated retinal detachments.
Unlike gas, patients are still able to see through clear silicone oil.
Positioning is less critical with silicone oil, therefore, it may be used in patients unable to position postoperatively (i.e. children).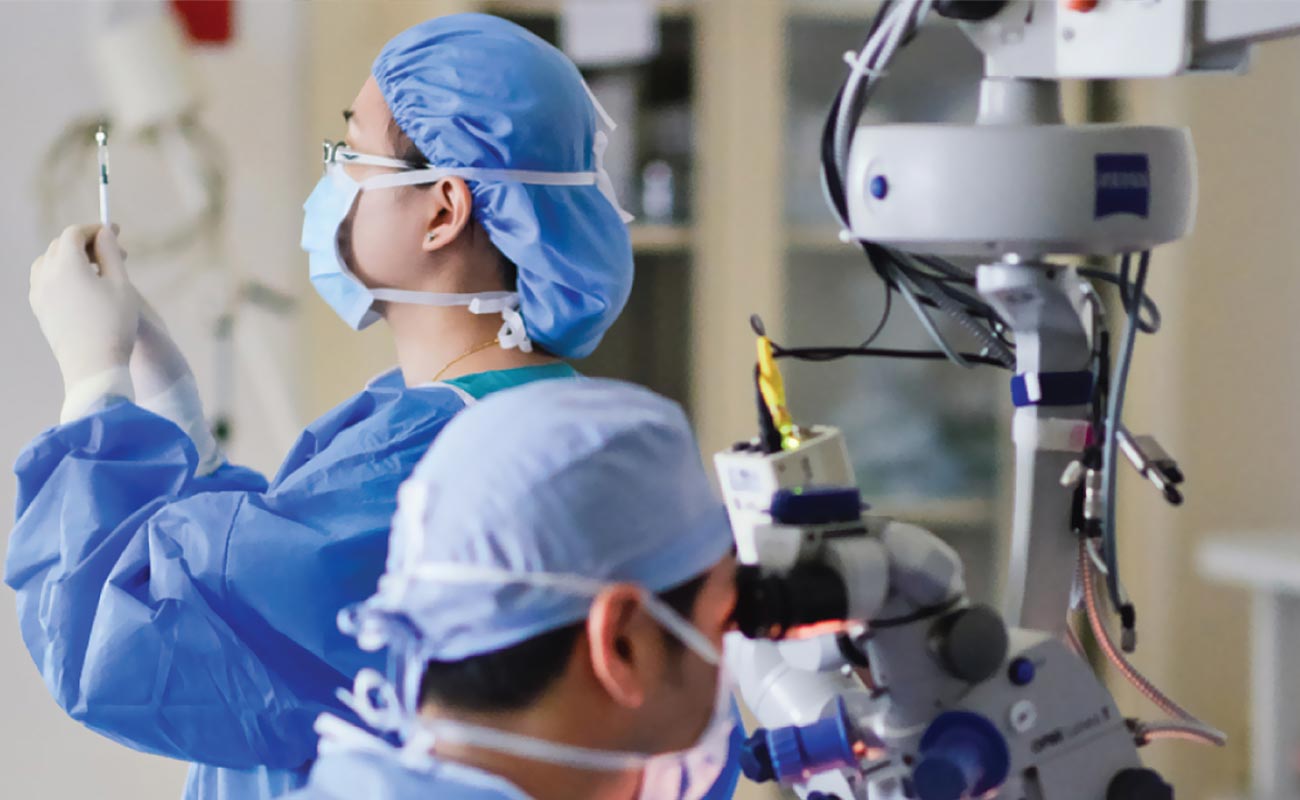
Silicone remains in the eye until it is removed (necessitating a second surgery at a later date).
Like gas, silicone oil can promote cataracts, cause glaucoma at times, and may damage the cornea but only if in contact.
Vitrectomies can be performed under local or general anesthesia. During vitrectomy surgery, your surgeon will first remove the blood-clouded vitreous gel from your eye. The vitreous tissue is then cut and removed one piece at a time and replaced with a special salt solution in order to maintain the eye's proper shape and pressure. The inside of the eye is illuminated, and the surgeon views the eye through a microscope.
In the case of a severely detached retina, it may be necessary to inject expandable gas into the eye during vitrectomy surgery. The expanding gas bubble pushes against the retina, helping it reattach. Patients must often lie face-down for two to four days until the gas bubble dissipates.

During vitrectomy surgery, a laser may be used to perform photocoagulation across the surface of the retina. This photocoagulation helps to prevent the formation of scar tissue and bleeding, and may also prevent the future growth of abnormal blood vessels.
Possible serious problems after this surgery include:
One of the main uses of vitrectomy is to treat vitreous hemorrhage. This surgery can have serious risks. So some doctors may want to wait up to a year before they do surgery. This delay lets them see if the vitreous gel will clear on its own.
Surgery may be done sooner if vitreous hemorrhage is causing severe vision loss or is preventing treatment of severe retinopathy. Long-term results may be better if surgery is done soon.
There are a few ways to repair a retinal detachment. Your eye doctor can help you understand which might be the best option for you.
Side effects
Vitrectomy complications range from having no improvement in your vision to permanent vision loss, though the majority of vitrectomy surgeries are successful. Vitrectomy-related complications are on the decline as a result of improved surgical techniques.
About 82 percent of vitrectomy patients experience significant improvements in vision after the surgery. Of the 18 percent of patients who experience vitrectomy complications, 9 percent have no improvement in their vision, and 9 percent experience permanent vision loss.
Neovascular glaucoma, one of the vitrectomy complications that can occur, causes permanent blindness in about 3 percent of vitrectomy patients. Neovascular glaucoma occurs when new blood vessels grow in the eye, blocking the drainage ducts. This blockage prevents fluid from draining properly and causes a build-up of pressure in the eye.
The risk for developing vitrectomy complications varies, depending on whether or not other procedures are performed in conjunction with your vitrectomy.
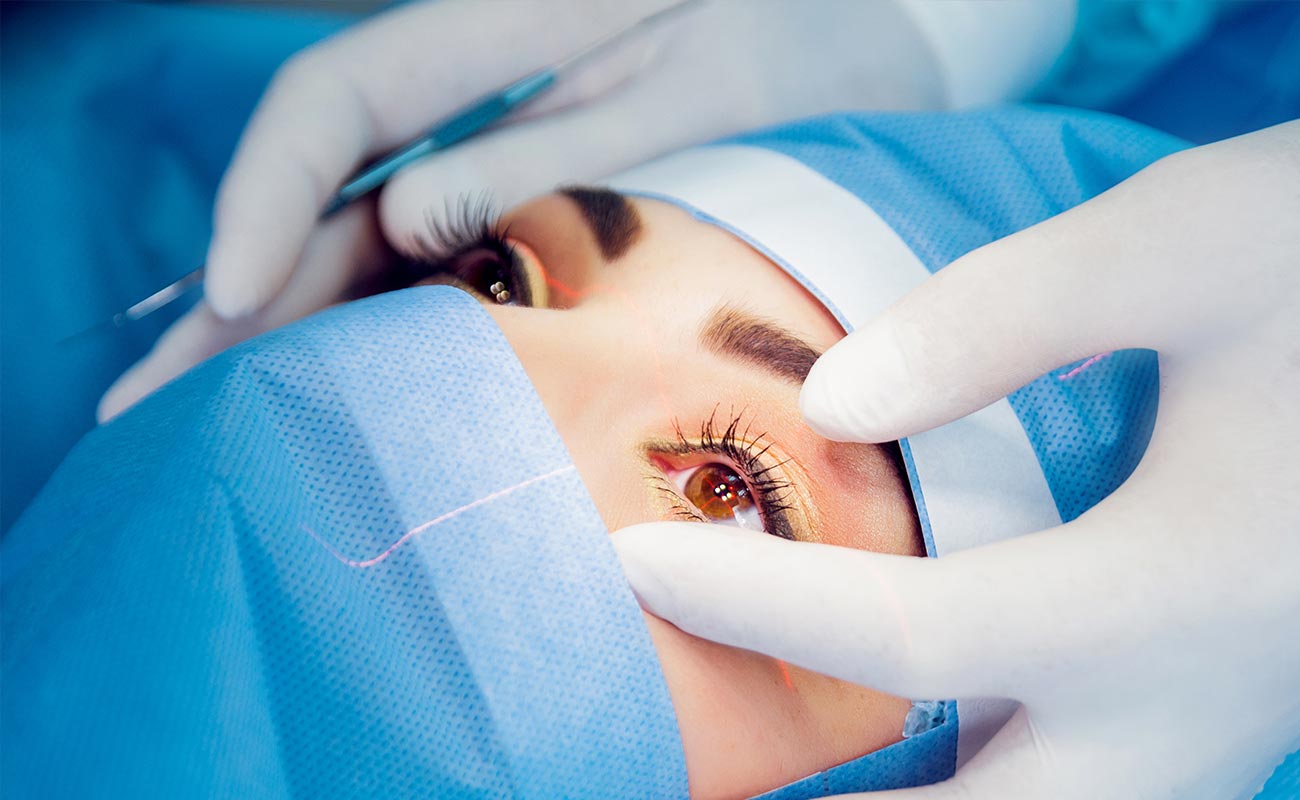
If you are required to lie face-down during your vitrectomy recovery, it is important that you follow your doctor's orders very carefully in order to avoid unnecessary vitrectomy complications
Surprisingly, a vitrectomy and removal of the vitreous has little effect on the health of the eye. The saline solution or gas bubble is gradually replaced by the eye’s own fluids (the aqueous humor).
If silicone oil is used as a vitreous substitute to help more serious conditions heal, a second procedure may be performed several months after surgery to remove the silicone oil. There may be some temporary swelling of the eyelids, bruising around the eye, and redness following the surgery, but these improve relatively quickly.
A mild sensation as if there is something in your eye is common following surgery, but severe pain is uncommon unless there is unusual inflammation or high eye pressure. Medicated eye drops are very important to help the eye heal.
As with most medical conditions, the healthier the eye is before surgery, the more likely the eye will heal quickly and the vision will improve. Some patients will note a decrease in vision for a few days following the procedure. Others, particularly if a gas bubble or silicone oil is used, may need weeks or even months for the vision to improve.
Severe complications are rare and anatomic success for vitrectomy is over 90% for many conditions. Advances in instrumentation, techniques, and understanding of diseases of the vitreous and retina have made vitrectomy and retina surgery more successful.
Surgery for diseases that were once incurable, such as macular hole, is now routinely performed with excellent results. The list of indications for vitreous surgery continues to grow. The ability to directly work on or near the retina holds great promise for the future, not only to prevent vision loss, but to restore and enhance our ability to see.
webmd.com, asrs.org, myeyeworld.com, docshop.com, allaboutvision.com.
Submit Comment