Thyroid cancer
Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer, and can spread to other areas of the body. To learn more about how cancers start and spread.
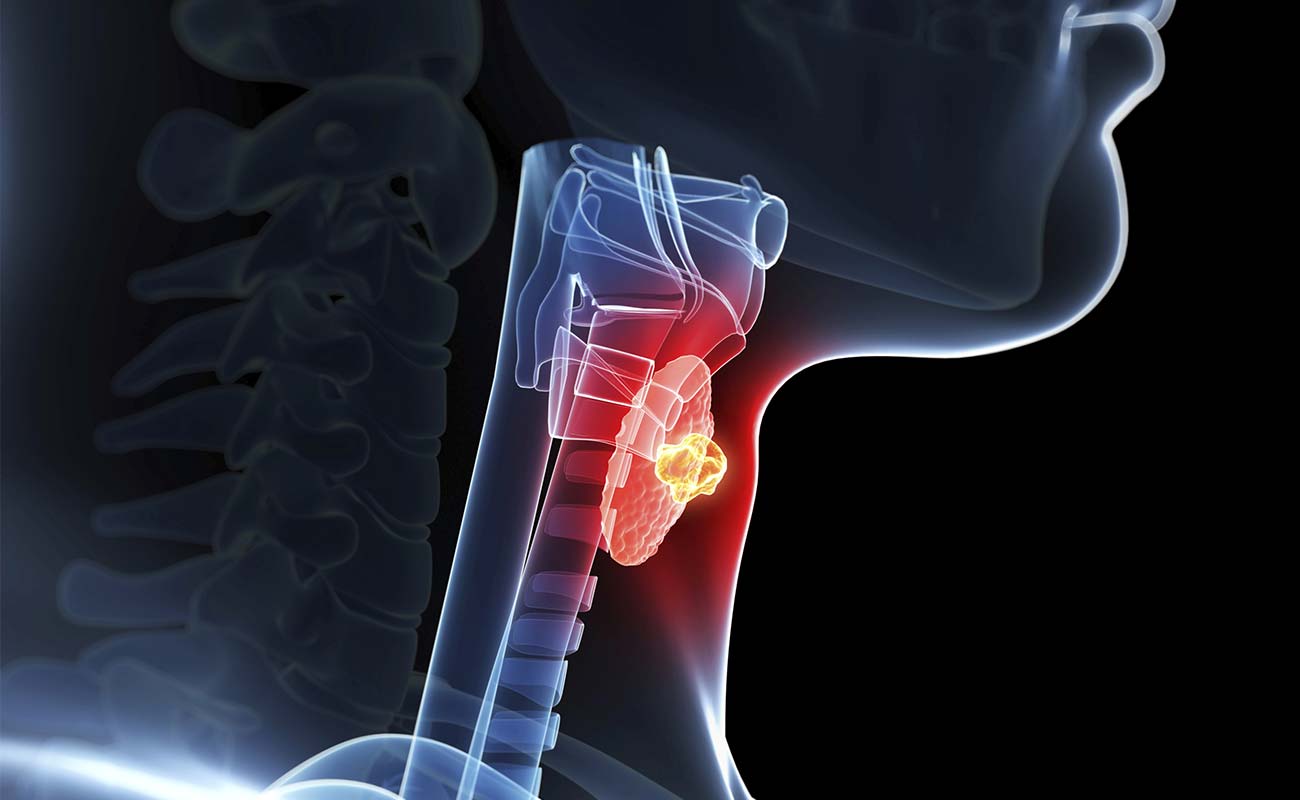
Thyroid cancer starts in the thyroid gland. To understand thyroid cancer, it helps to know about the normal structure and function of the thyroid gland.
Symptoms
- A lump in the neck, sometimes growing quickly
- Swelling in the neck
- Pain in the front of the neck, sometimes going up to the ears
- Hoarseness or other voice changes that do not go away
- Trouble swallowing
- Trouble breathing
- A constant cough that is not due to a cold
If you have any of these signs or symptoms, talk to your doctor right away. Many of these symptoms can also be caused by non-cancerous conditions or even other cancers of the neck area. Lumps in the thyroid are common and are usually benign. Still, if you have any of these symptoms, it’s important to see your doctor right away so the cause can be found and treated, if needed.
Causes
Thyroid cancer occurs when cells in your thyroid undergo genetic changes (mutations). The mutations allow the cells to grow and multiply rapidly. The cells also lose the ability to die, as normal cells would. The accumulating abnormal thyroid cells form a tumor. The abnormal cells can invade nearby tissue and can spread throughout the body.
Types of thyroid cancer
The type of thyroid cancer you have determines treatment and prognosis. Types of thyroid cancer include:
- Papillary thyroid cancer. The most common form of thyroid cancer, papillary cancer arises from follicular cells, which produce and store thyroid hormones. Papillary thyroid cancer can occur at any age, but most often it affects people ages 30-50.
- Follicular thyroid cancer. Follicular cancer also arises from the follicular cells of the thyroid. It usually affects people older than age 50. Hurthle cell cancer is a rare and potentially more aggressive type of follicular thyroid cancer.
- Medullary thyroid cancer. Medullary thyroid cancer begins in thyroid cells called C cells that produce the hormone calcitonin. Elevated levels of calcitonin in the blood can detect medullary thyroid cancer at a very early stage. Certain genetic syndromes increase the risk of medullary thyroid cancer, although this genetic link is uncommon.
- Anaplastic thyroid cancer. Anaplastic thyroid cancer is a rare and rapidly growing cancer that is very difficult to treat. Anaplastic thyroid cancer typically occurs in adults age 60 or older.
- Thyroid lymphoma. Thyroid lymphoma is a rare form of thyroid cancer that begins in the immune system cells in the thyroid and grows very quickly. Thyroid lymphoma typically occurs in older adults.
Diagnosis
For most types of cancer, a biopsy is the only sure way for the doctor to know whether an area of the body has cancer. In a biopsy, the doctor takes a small sample of tissue for testing in a laboratory. If a biopsy is not possible, the doctor may suggest other tests that will help make a diagnosis.
Your doctor may consider these factors when choosing a diagnostic test:
- The type of cancer suspected
- Your signs and symptoms
- Your age and medical condition
- The results of earlier medical tests
The list below describes options for diagnosing this type of cancer. Not all tests listed below will be used for every person.
- Physical examination. The doctor will feel the neck, thyroid, throat, and lymph nodes (the tiny, bean-shaped organs that help fight infection) in the neck for unusual growths or swelling. If surgery is recommended, the larynx may be examined at the same time with a laryngoscope, which is a thin, flexible tube with a light.
- Blood tests. There are several types of blood tests that may be done during diagnosis and to monitor the patient during and after treatment. This includes tests called tumor marker tests. Tumor markers are substances found at higher-than-normal levels in the blood, urine, or body tissues of some people with cancer.
- Thyroid hormone levels. As explained in the Introduction, thyroid hormones regulate a person’s metabolism. The doctor will use this test to find out the current levels of the thyroid hormones triiodothyronine (T3) and thyroxine (T4) in the body.
- Thyroid-stimulating hormone (TSH). This blood test measures the level of TSH, a hormone produced by the pituitary gland near the brain. If the body is in need of thyroid hormone, the pituitary gland releases TSH to stimulate production.
- Tg and TgAb. Thyroglobulin (Tg) is a protein made naturally by the thyroid as well as by differentiated thyroid cancer. After treatment, there should be very low levels of thyroglobulin in the blood since the goal of treatment is to remove all thyroid cells. If Tg is rising after surgery and/or radioactive iodine, it may be a sign of more cancer. A tumor marker test may be done to measure the body’s Tg level before, during, and/or after treatment. There is also a test for thyroglobulin antibodies (TgAb), which are proteins produced by the body to attack thyroglobulin that occur in some patients. If TgAb is found, it is known to interfere with the results of the Tg level test.
- Medullary type-specific tests. If MTC is a possibility, the doctor will order tumor marker tests to check for high calcitonin and carcinoembryonic antigen (CEA) levels. The doctor should also recommend a blood test to detect the presence of RET proto-oncogenes (see Risk Factors), particularly if there is a family history of MTC.
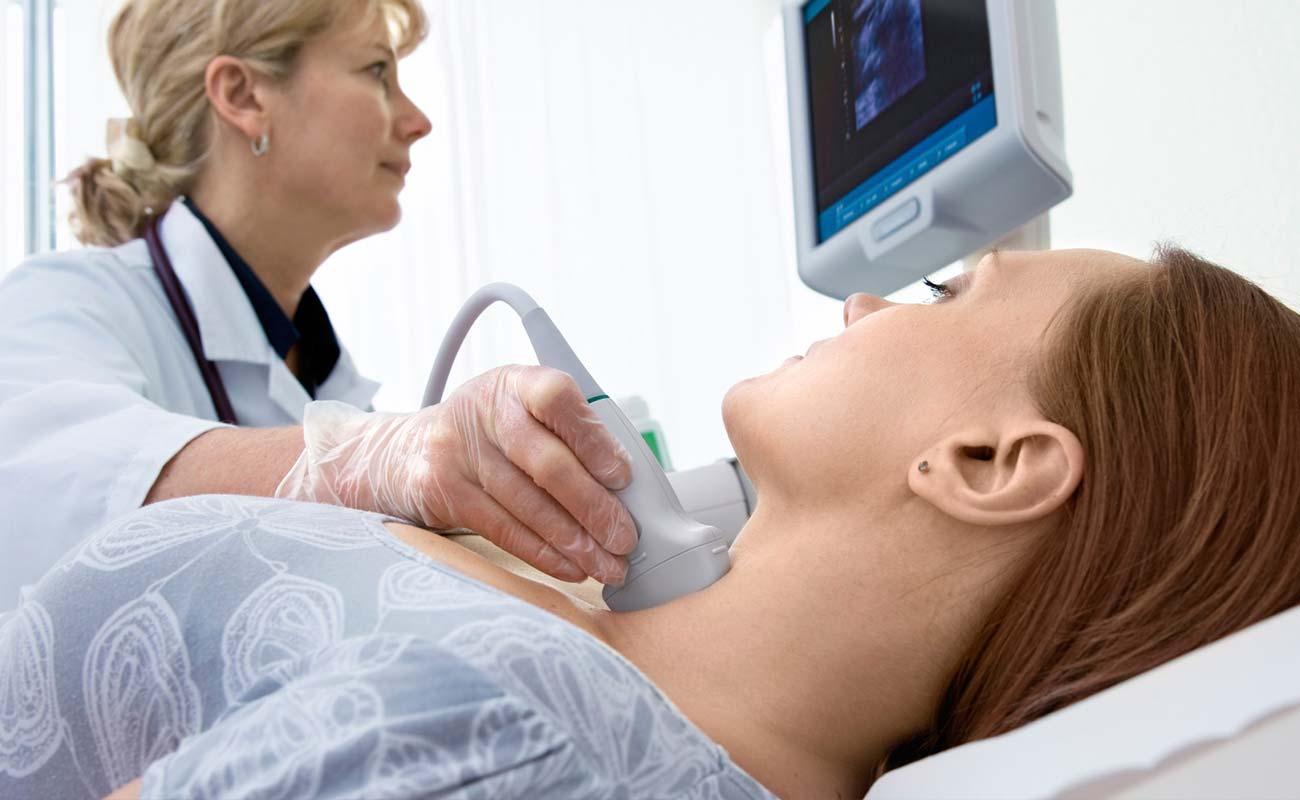
- Ultrasound. An ultrasound uses sound waves to create a picture of the internal organs. An ultrasound wand or probe is guided over the skin of the neck area. High-frequency sound waves create a pattern of echoes that show the doctor the size of the thyroid gland and specific information about any nodules, including whether a nodule is solid or a fluid-filled sac called a cyst.
- Biopsy. A biopsy is the removal of a small amount of tissue for examination under a microscope. Other tests can suggest that cancer is present, but only a biopsy can make a definite diagnosis. The way to determine whether a nodule is cancerous or benign is through a biopsy. During this procedure, the doctor removes cells from the nodule that are then examined by a cytopathologist. A cytopathologist is a doctor who specializes in analyzing cells and tissue to diagnose disease. This test is often done with the help of ultrasound.
A biopsy for thyroid nodules will be done in 1 of 2 ways:
- Fine needle aspiration. This procedure is usually performed in a doctor’s office or clinic. It is an important diagnostic step to find out if a thyroid nodule is benign or cancerous. A local anesthetic may be injected into the skin to numb the area before the biopsy. The doctor inserts a thin needle into the nodule and removes cells and some fluid. The procedure may be repeated 2 or 3 times to get samples from different areas of the nodule. The report is created by the cytopathologist. A pathologist is a doctor who specializes in interpreting laboratory tests and evaluating cells, tissues, and organs to diagnose disease. The test can be positive, meaning there are cancerous cells, or negative, meaning there are no cancerous cells. The test can also be undetermined, meaning it is not clear whether cancer is there. Unfortunately, it can be possible to miss the targeted area.
- Surgical biopsy. If the needle aspiration biopsy is not clear, the doctor may suggest a biopsy in which the nodule and possibly the affected lobe of the thyroid will be removed. This procedure is usually done under general anesthesia. It may also require a hospital stay.
- Molecular testing of the tumor. Your doctor may recommend running laboratory tests on a tumor sample to identify specific genes, proteins, and other factors unique to the tumor. Results of these tests will help decide whether your treatment options include a type of treatment called targeted therapy (see Treatment Options).
- Radionuclide scanning. This test may also be called a whole-body scan. This scan will either be done using I-131 or I-123. It is used most often to learn more about a thyroid nodule. In this test, the patient swallows a very small, harmless amount of radioactive iodine, which is absorbed by thyroid cells. This makes the thyroid cells appear on the scan image, allowing the doctor to see differences between those cells and other body structures.
- X-ray. An x-ray is a way to create a picture of the structures inside of the body, using a small amount of radiation. For instance, a chest x-ray can help doctors determine if the cancer has spread to the lungs.
- Computed tomography (CT or CAT) scan. A CT scan creates a 3-dimensional picture of the inside of the body using x-rays taken from different angles. A computer then combines these images into a detailed, cross-sectional view that shows any abnormalities or tumors. A CT scan can also be used to measure the tumor’s size. Sometimes, a special dye called a contrast medium is given before the scan to provide better detail on the image. This dye can be injected into a patient’s vein or given as a pill to swallow.
CT scans are often used in patients with thyroid cancer to examine parts of the neck that cannot be seen with ultrasound (see above). Also, CT scans of the chest may be needed to look to see if thyroid cancer has spread. CT scans of the abdomen may be used to see if thyroid cancer has spread to the liver or other sites. Patients with the hereditary form (see Risk Factors) of medullary thyroid cancers may be at risk for developing other types of endocrine tumors in the abdomen; these patients may also have a CT scan of the abdomen.
- Positron emission tomography (PET) or PET-CT scan. A PET scan is usually combined with a CT scan (see above), called a PET-CT scan. However, you may hear your doctor refer to this procedure just as a PET scan. A PET scan is a way to create pictures of organs and tissues inside the body. A small amount of a radioactive sugar substance is injected into the patient’s body. This sugar substance is taken up by cells that use the most energy. Because cancer tends to use energy actively, it absorbs more of the radioactive substance. A scanner then detects this substance to produce images of the inside of the body.
After diagnostic tests are done, your doctor will review all of the results with you. If the diagnosis is thyroid cancer, these results also help the doctor describe the cancer. This is called staging.
Treatment
The goal of treatment for thyroid cancer is to get rid of the cancer cells in your body. How this is done depends on your age, the type of thyroid cancer you have, the stage of your cancer, and your general health.
Most people have surgery to remove part or all of the thyroid gland. Sometimes a suspicious lump or nodule has to be surgically removed before you will know if you have cancer or not.
After surgery, you may need treatment with radioactive iodine to destroy any remaining thyroid tissue. When you no longer have all or part of your thyroid gland, you will probably need to take thyroid hormone medicines for the rest of your life. These medicines replace necessary hormones that are normally made by the thyroid gland and prevent you from having hypothyroidism-too little thyroid hormone.
Initial treatment
The treatment for thyroid cancer may include:
- Surgery to remove the part of the thyroid gland that contains cancer. Removing one part (lobe) is called a lobectomy. Removing both lobes is called a total thyroidectomy. Removing all but a very small part of the thyroid is called a near-total thyroidectomy. Lymph nodes may also be removed during surgery.
- Radioactive iodine, which is used after surgery to destroy any remaining thyroid tissue. After you have your thyroid surgically removed, you may have to wait several weeks before having radioactive iodine treatment to destroy any remaining thyroid tissue. During the waiting period, you may have symptoms of hypothyroidism such as fatigue, weakness, weight gain, depression, memory problems, or constipation.
- Thyroid-stimulating hormone (TSH) suppression therapy. TSH suppression therapy reduces the TSH in your body, which may help prevent the growth of any remaining cancer cells.
If thyroid cancer is advanced when it is diagnosed, initial treatment may also include chemotherapy or radiation therapy.
Ongoing treatment
After treatment for thyroid cancer, you may need to take thyroid hormone medicine for the rest of your life to replace the hormones that your body no longer makes. You will also need follow-up visits with your doctor every 6 to 12 months. In addition to scheduling regular visits, be sure to call your doctor if you notice another lump in your neck or if you have trouble breathing or swallowing.
At your follow-up visits, your doctor may order a blood test to measure your thyroid-stimulating hormone (TSH) level. This test helps your doctor know if you are taking the right amount of thyroid hormone medicine. Your doctor may order other tests, such as a radioiodine scan, X-rays, or a CT scan.
Side effects of treatment
The side effects of surgery for thyroid cancer are usually mild and last a couple of days. Your doctor will talk to you about medicine you can take if you are having pain. You will likely need to take thyroid hormone medicine for the rest of your life to replace the hormones that your body no longer makes.
The most important side effect of radioactive iodine therapy (RAI) is that you will become radioactive for a period of time. Your doctor will give you written instructions to follow to prevent exposing others to radiation. For more information, see Radioactive Iodine.
Thyroid hormone therapy rarely causes side effects when you have the right dose. Too much or too little thyroid hormone can cause side effects.
Taking high doses of thyroid hormone may cause a rapid or irregular heartbeat. High doses taken over time may also cause weakness in your bones (osteoporosis).
Home treatment may help you manage your side effects.
Treatment if the condition gets worse
Thyroid cancer may come back (recur). If thyroid cancer does recur, it may be found during a physical exam, on an ultrasound, or as a result of increasing thyroglobulin levels. Unlike other types of recurrent cancer, recurrent thyroid cancer is often cured, especially if it has spread only to the lymph nodes in the neck.
Recurrent thyroid cancer or thyroid cancer that has spread (metastasized) to other parts of the body may be treated with surgery, radioactive iodine, radiation, or chemotherapy.
Clinical trials
Your doctor may talk to you about being in a clinical trial. For some people with thyroid cancer, taking part in a clinical trial may be the best treatment choice. Clinical trials for thyroid cancer are looking at targeted therapy with tyrosine kinase inhibitors.
Palliative care
Palliative care is a kind of care for people who have a serious illness. It's different from care to cure your illness. Its goal is to improve your quality of life-not just in your body but also in your mind and spirit.
You can have palliative care along with treatment to cure your illness. You can also have it if treatment to cure your illness no longer seems like a good choice.
Palliative care providers will work to help control pain or side effects. They may help you decide what treatment you want or don't want. And they can help your loved ones understand how to support you.
If you're interested in palliative care, talk to your doctor.
For more information, see the topic Palliative Care.
Sources: endocrineweb, mayoclinic.org, mayoclinic.org, cancer.net, webmd




Submit Comment