Cervical mucus is a jelly-like substance produced by tiny glands in the cervix called cervical crypts. It has a protective function and may prevent bacteria from getting into the uterine cavity. The mucus changes predictably and cyclically during the menstrual cycle.
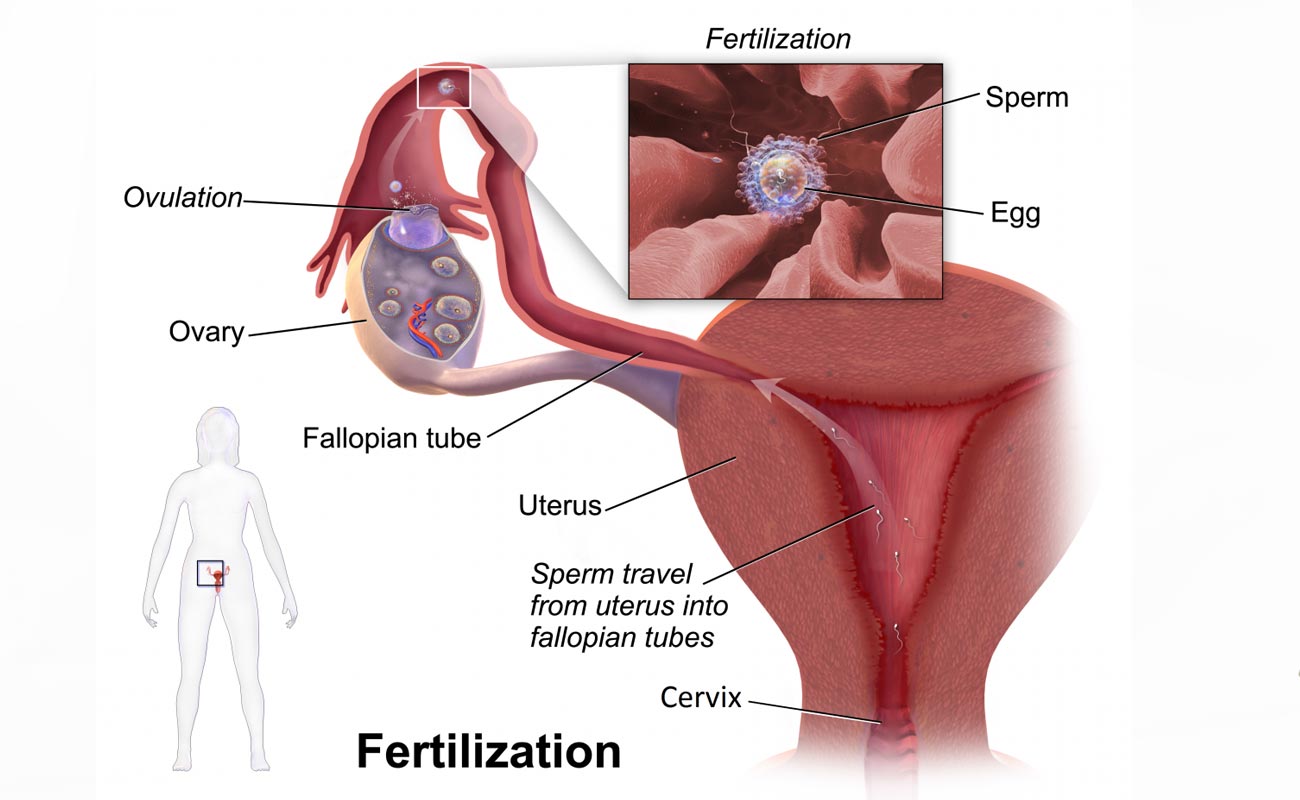
During the first half of the cycle before ovulation, when the hormone estrogen is produced in ever increasing amounts, the mucus made by the cervical glands becomes watery and copious. Sperm can penetrate the watery mucus easily, and when intercourse takes place, they swim through it into the uterus.
After ovulation the quality of the mucus changes because the corpus luteum of the ovary now starts to make the hormone progesterone. Mucus produced under the influence of progesterone is thicker, stickier and its quantity is reduced. Sperm cannot swim through this mucus, and it forms a barrier to sperm entry into the uterine cavity.

A major player in a couple’s ability to get pregnant is the woman’s cervical mucus. Cervical mucus is a jelly like substance produced by minute glands in the cervical canal. The cervical mucus consistency varies through a woman’s cycle.
The first few days following menstruation, there will be little or no discharge present.
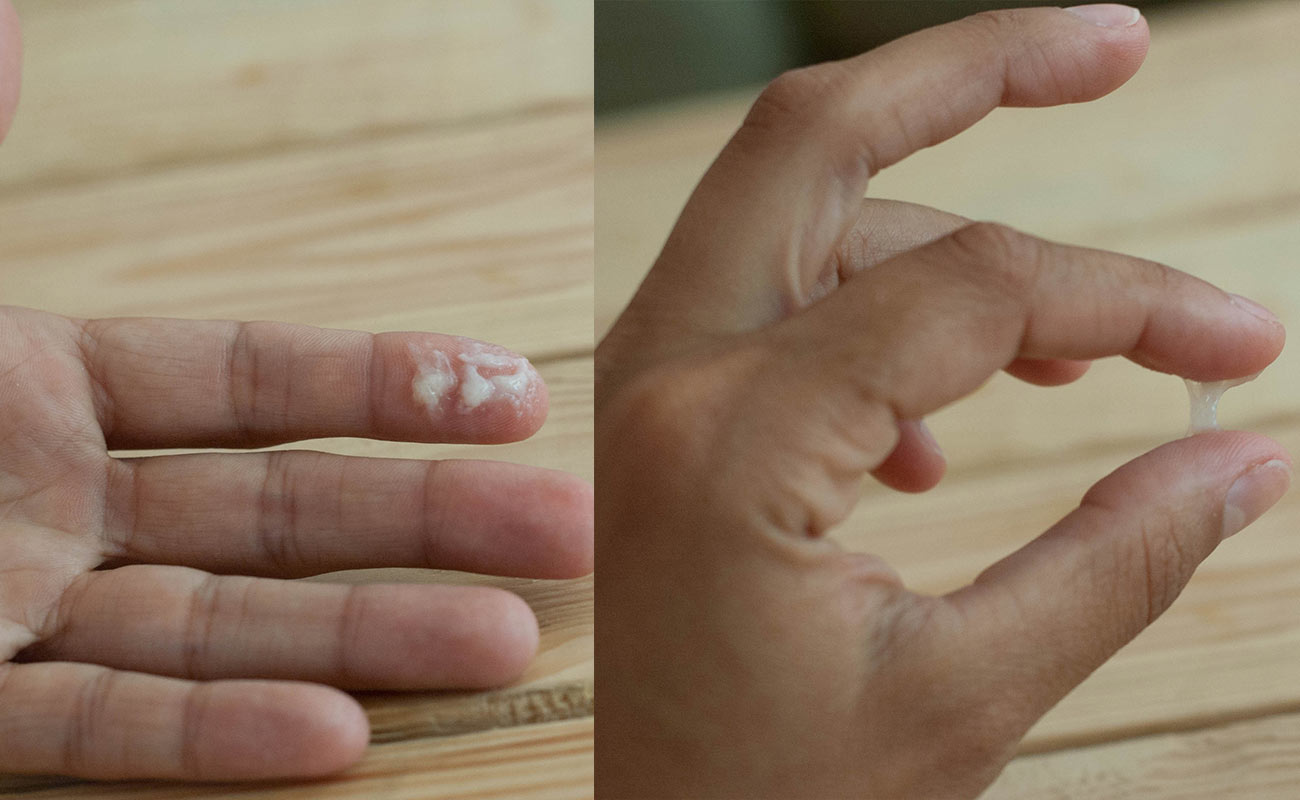
The first discharge that does appear should be moist or sticky and should be white or cream in color. In the finger test, the mucus should break easily.
At this stage, mucus resembles egg whites. It is the thinnest, clearest and most abundant at this point in the cycle. During this phase, the sperm’s survival rate is higher. It can survive in cervical mucus for up to 72 hours, a significantly longer time than during the rest of the cycle.
After ovulation, there is a marked change in mucus appearance. It returns to the sticky stage (does not stretch during finger test) and there is again a feeling of dryness around the vulva.
Cervical mucus is supposed to protect the sperm on their journey and help to keep them safe. The best cervical mucus for protecting sperm is known as “egg white cervical mucus”. This cervical mucus is clear, stretchy, and has the consistency of egg whites. Sometimes however, cervical mucus turns “hostile”, and actually hurts the sperm instead of protecting it. When a woman’s cervical mucus is hostile, that means it is too thick to allow the sperm to penetrate the cervix, and the cervical mucus is actually doing more harm than good.
Suboptimal mucus conditions that effect sperm survival and penetration ("hostile mucus") include:
There are several different causes of hostile cervical mucus. One of the most common causes of hostile cervical mucus is a poor diet. When a woman doesn’t get enough water, or consumes too much dairy, her cervical mucus can quickly become hostile. Another reason for hostile cervical mucus can be medications. One of the most common fertility drugs, Clomid, can be responsible for creating hostile cervical mucus in many women. Other common over the counter drugs, such as antihistamines can also create hostile cervical mucus.
Treatment will really depend on the cause of the hostile cervical mucus and if there are other fertility factors.
In the case of less than fertile quality cervical mucus – assume there is no infection or anti-sperm antibodies – it may be possible to treat it using fertility friendly lubricants.
Or, if the lack of fertile quality mucus is a side effect of a medication, that medication may need to be discontinued to replaced with something else. (Never stop any medication without speaking to your doctor first.)
Another possible treatment for dry or sticky fertile mucus is with Ethinyl estradiol, a form of synthetic estrogen. When used in the short-term, it may improve production of cervical mucus and improve its fertile quality.
A popular over-the-counter treatment of poor cervical mucus quality is with guaifenesin, a medication most commonly found in cough syrups. It works by increasing and thinning mucus in the body.
If the cause of cervical mucus hostility is an infection, treating the infection with antibiotics or antifungals may be required.
If anti-sperm antibodies are present, IVF may be required. The research is unclear whether IUI significantly improves pregnancy rates in the cases of immunological fertility problems.
There’s some evidence that B-vitamins, especially folic acid and B-6 may help improve cervical fluid quality. The evidence isn’t very strong, though.
(Note however that folic acid is essential to fertility and healthy early pregnancy. Also, at least one study found that women who took a daily multivitamin were less likely to experience ovulatory infertility.)
There are a number of natural remedies proposed online, many with very little or no evidence to back them up.
Dietary suggestions include reducing dairy product consumption, decreasing carbohydrates, and changing the diet to be more alkaline (rather than acidic.) There’s no evidence for these suggestions.
Many websites suggest drinking more water to improve cervical mucus quality. If you are seriously dehydrated, it could affect your cervical fluids. But in most cases, drinking more water isn’t going to make a difference.

The post-coital test is performed as closely as possible to the time of ovulation when the cervical mucus is receptive to sperm migration.At any other time during your cycle, cervicalmucus is hostile to sperm.The following instructions should be followed, as closely as possible in preparation for the post-coital test:
1. The timing of ovulation will be determined by your doctor and you will be told to have intercourse around ovulation time and about 4-10 hours before the PCT.
2. Intercourse should take place according to your normal practice at the times specified by your doctor or Coordinating Sister.
3. Have a shower before you come in for your test.
4. Report to your doctor or Concept Fertility Centre for the test at the time you were instructed to do so.
verywell.com, drmalpani.com, drdaiter.com, babyhopes.com, conceiveeasy.com, myfertility.ca
Submit Comment