Arthroscopy is a procedure for diagnosing and treating joint problems. A surgeon inserts a narrow tube attached to a fiber-optic video camera through a small incision — about the size of a buttonhole. The view inside your joint is transmitted to a high-definition video monitor.
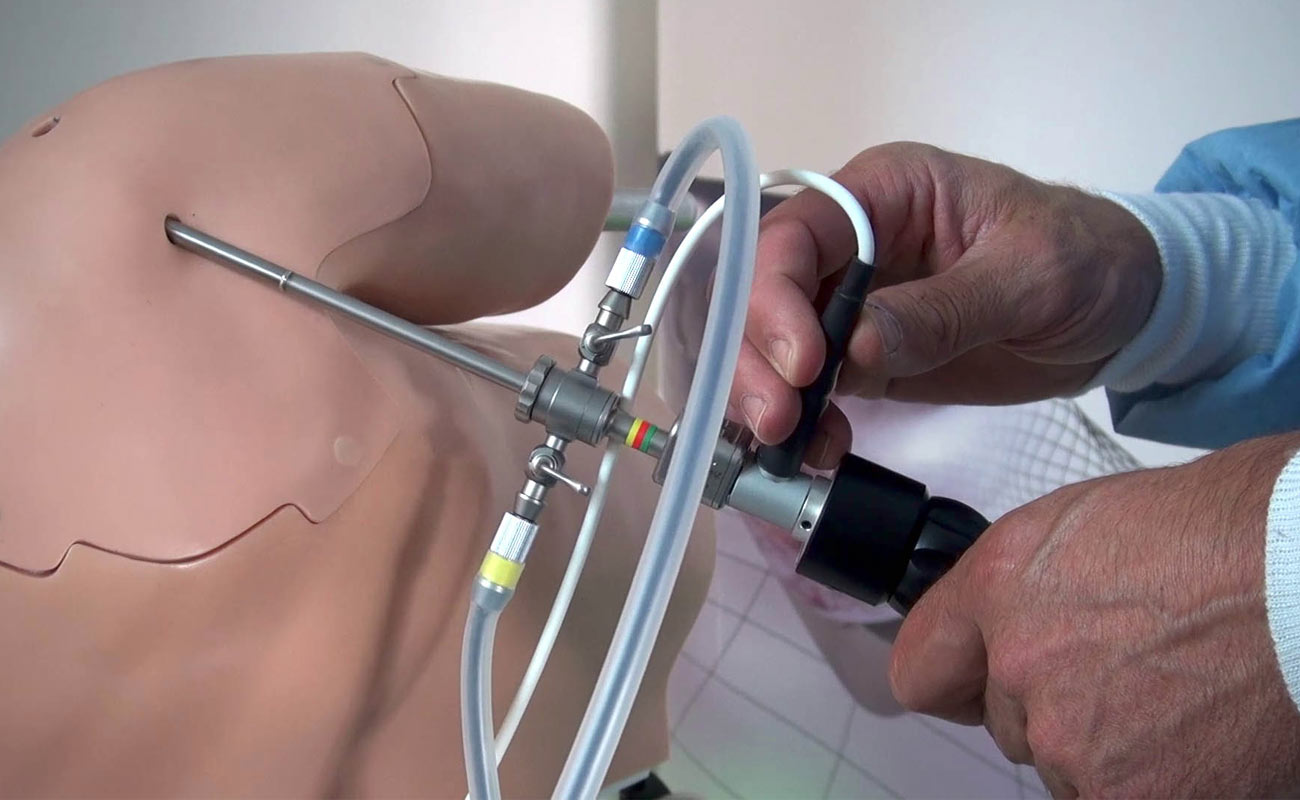
Surgeons can even repair some types of joint damage during arthroscopy, with pencil-thin surgical instruments inserted through additional small incisions.
Arthroscopy is a highly common procedure and can diagnose joint problems such as joint pains and stiffness, swelling of the joints and joints ‘popping’ out of position.
This is very common in sportsmen and those with an underlying condition such as osteoarthritis. It most commonly affects the:
Arthroscopy is essentially a procedure during which no blood loss is expected and generally has few complications. The underlying health of the patient is considered when determining who is a candidate for arthroscopy. Most importantly, the patient should be able tolerate the anesthetic that is used during the procedure. A person's heart, kidney, liver, and lung function should be adequate. If there are existing problems such as heart failure or emphysema, these should be optimized as possible prior to surgery. Patients who are on anticoagulants (blood thinners) should have these medications carefully adjusted prior to surgery. Other medical problems should also be controlled prior to surgery, such as diabetes and high blood pressure.
Preoperative evaluation of a patient's health will generally include a physical examination, blood tests, and a urinalysis. Patients who have a history of heart or lung problems and generally anyone over the age of 50 will usually be asked to obtain an electrocardiogram (EKG) and a chest X-ray. Any signs of ongoing infection in the body usually postpones arthroscopy, unless it is being done for possible infection of the joint in question.
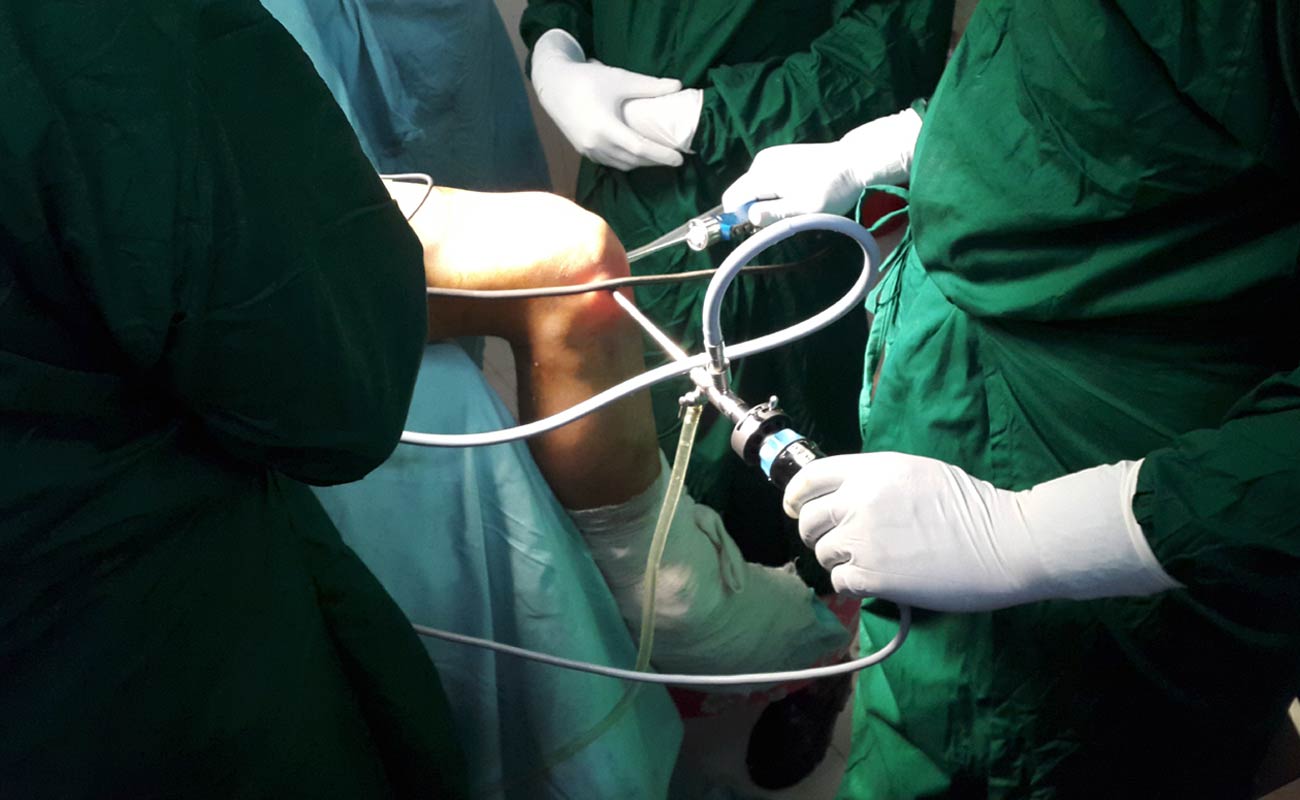
An arthroscopy is usually carried out under general anaesthetic, although occasionally it can be performed under spinal anaesthesia, or with local anaesthetic. Your anaesthetist will explain which type of anaesthetic is most suitable for you. In some cases, you may be able to express a preference.
If you have a local anaesthetic, your joint will be numbed so you do not feel any pain. However, you may still feel some sensations during the procedure, such as a mild tugging, as the surgeon works on the joint.
Antibacterial fluid is used to clean the skin over the affected joint and a small incision, a few millimetres long, is made so the arthroscope can be inserted. One or more additional incisions will also be made so that an examining probe or other fine surgical instruments can be inserted.
The surgeon may fill the joint with a sterile fluid to expand it and make it easier to view. They will be able to see inside your joint using an eyepiece or a video screen. If possible, during the procedure, they will repair any damaged areas and remove any unwanted tissue.
Your surgeon will then examine the inside of the joint using the arthroscope and, if necessary, remove or repair any problems areas using surgical instruments inserted through the additional incisions.
After the procedure, the arthroscope and any attachments are removed, along with any excess fluid from the joint. The incisions are usually closed using special tape or stitches and covered with a sterile dressing.
Complications are rare, but no procedure is completely free of risk. If you are planning to have an arthroscopy, your doctor will review a list of possible complications, which may include:
Factors that may increase the risk of complications include:

After arriving home, contact your doctor if any of the following occurs:
mayoclinic.org, medicinenet.com, healthline, nhs.uk
Submit Comment