The most advanced form in a series of conditions all related to the same disease, Alopecia Universalis (AU) is characterized by total a loss of body hair. A member of the group of hair loss conditions called Alopecia Areata, the only difference between Alopecia Universalis and its variants is the extent of hair loss.
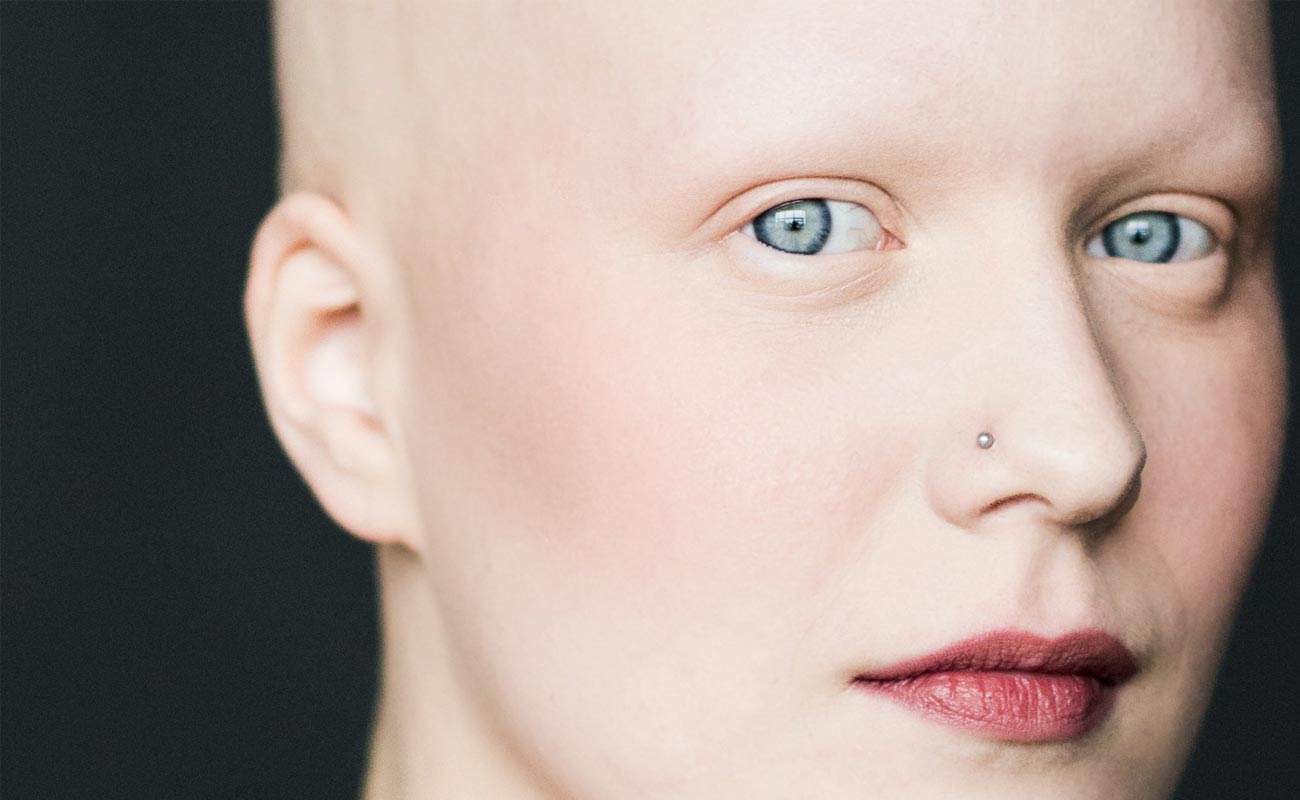
Although the exact cause of AU is unknown, it is thought to be an autoimmune condition in which an affected person's immune system mistakenly attacks the hair follicles. Roughly 20% of affected people have a family member with alopecia, suggesting that genetic factors may contribute to the development of AU. There is currently no cure for AU, but sometimes hair regrowth occurs on its own, even after many years.

Normally, sufferers are otherwise healthy, but are more likely than the general population to experience thyroid disease and vitiligo (patchy loss of skin color). Those with vitiligo may eventually develop AU over time. Many individuals with Alopecia Universalis are born with some hair but begin losing it very quickly. The disorder is inherited as an autosomal recessive trait. It is caused by a mutation in a gene dubbed HR in chromosome band 8p21.2 — the human version of the gene that is responsible for hairlessness in mice.
Is the “hairless” gene only found in people with alopecia universalis? Most likely. Based on the known research, we can safely assume that only individuals with this rare and severe form of alopecia areata carry the gene. Unfortunately, there have not been enough studies to verify that this is true of all those afflicted. Aside from genetic tendencies, the contributing causes of Alopecia Universalis are not known.
As lack of body hair leaves areas like the scalp, eyes and nasal cavity particularly vulnerable, it is important that those with Alopecia Universalis take extra care to protect themselves from the sun, bacteria and other potentially harmful elements.
According to the National Alopecia Areata Foundation, fingernails and toenails can also be affected. Symptoms in the nails can range from pinprick-like indentations to severe distortion of the entire nail. Alopecia Universalis may be acute and short-lived or remain permanently. Regrowth is always a possibility, even for those with 100% hair loss over many years. However, it is not possible to predict when regrowth will occur.

The condition occurs when white blood cells attack the cells in hair follicles, causing them to shrink and dramatically slow down hair production. It is unknown precisely what causes the body's immune system to target hair follicles in this way.
While scientists are unsure why these changes occur, it seems that genetics are involved as alopecia areata is more likely to occur in a person who has a close family member with the disease. One in five people with the disease has a family member who has also developed alopecia areata.
Other research has found that many people with a family history of alopecia areata also have a personal or family history of other autoimmune disorders, such as atopy (a disorder characterized by a tendency to be "hyperallergic"), thyroiditis, and vitiligo.
Despite what many people think, there is very little scientific evidence to support the view that alopecia areata is caused by stress. Extreme cases of stress could potentially trigger the condition, but most recent research points toward a genetic cause.
Doctors are usually able to diagnose alopecia areata fairly easily by examining symptoms. They might look at the degree of hair loss and examine hairs from affected areas under a microscope.
If, after an initial clinical examination, the doctor is not able to make a diagnosis, they can perform a skin biopsy. If they need to rule out other autoimmune diseases, they might perform a blood test.
As the symptoms of alopecia areata are so distinctive, making a diagnosis is usually quick and straightforward.

There are a range of treatments for AA, but none are effective for everyone and some people with AA don't respond to any treatment. Because some of the available treatments have a high risk of side effects, they are often not used for children.
The most common AA treatment involves the use of corticosteroids. Corticosteroid creams applied to the bald patches are popular with the average dermatologist, although this treatment approach is only successful for the very mildest cases. A more potent approach is to inject corticosteroid solutions into the bald patches. This can work well for some people, but close monitoring is required to ensure that side effects, such as skin thinning at the site of injection, do not occur.
In extensive cases, systemic corticosteroids (those taken in pill or other form to affect your body) are used, though not continuously since they can cause significant side effects like bone thinning. But short-term "pulse therapy" often has good results.
More specialized treatment approaches involve the application of contact sensitizing chemicals to the skin. These cause an allergic reaction that can help promote hair growth. That may sound counterintuitive but it seems to work. A variety of experimental approaches are currently in laboratory and clinical trials. One group of drugs being tested are "biologics," which have bits of protein that interfere in a very specific way with the activity of immune cells. Biologics are injected systemically to damp down the immune activity and allow hair to regrow. The results of these trials are awaited with much interest.
Unfortunately, people with more extensive, long-term AA find the treatments currently available do not work well. For these individuals the only practical answer is a wig and lots of emotional support. It can be depressing not to have hair, especially for children, who don't want to be different from their classmates at school, and women. In North America and many other countries of the world, you can access a network of support agencies for people with AA.
onlymyhealth.com, rarediseases.info.nih.gov, naaf.org, hairlosstalk.com, medicalnewstoday.com, webmd.com
Submit Comment