Addison’s disease, also called hypoadrenalism or primary adrenal insufficiency, is a rare condition related to adrenal glands.

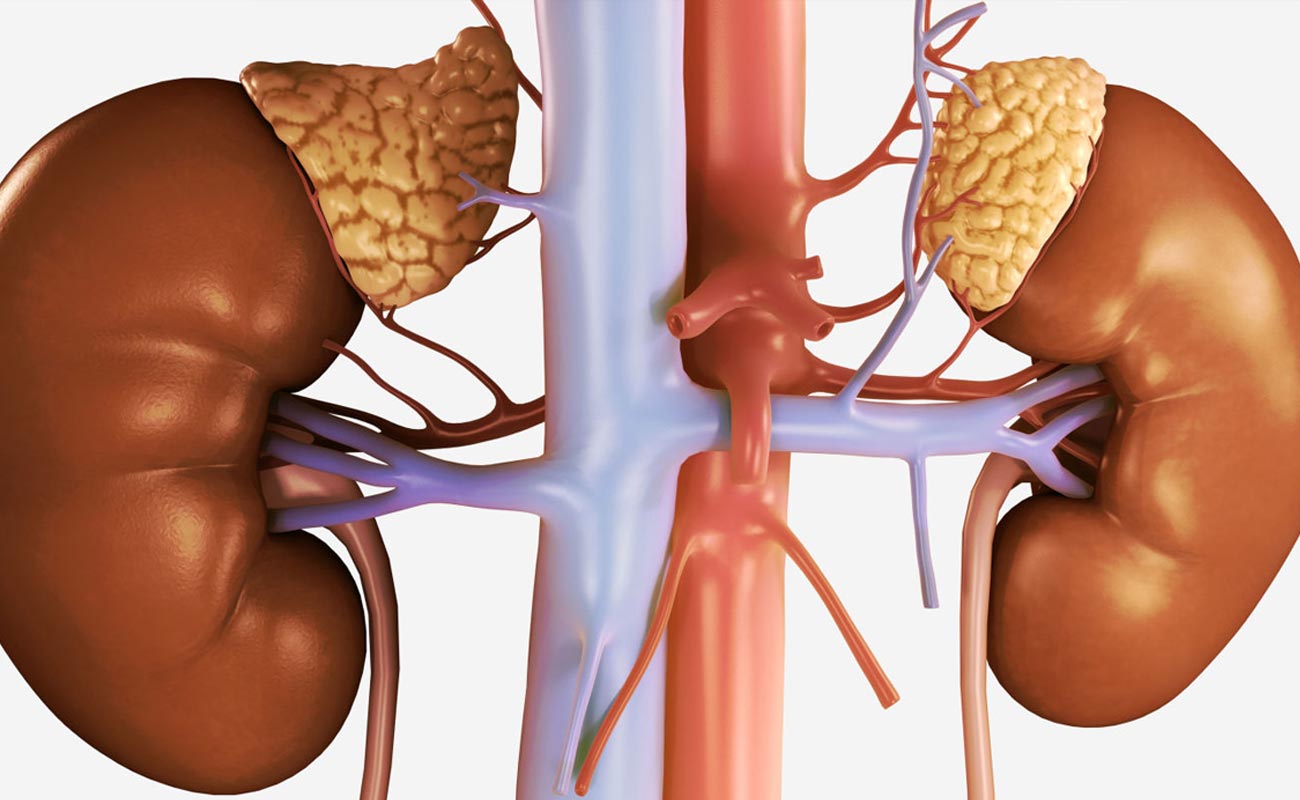
The adrenal glands are two small glands located above kidneys. These glands are the sources of two vital hormones: cortisol and aldosterone.
In those patients with Addison's disease, the adrenal glands are damaged so that less than normal cortisol and aldosterone are produced.
Addison's disease can affect all people in any walks of life. However, it is most common between the ages of 30 and 50. Also, it is more prevalent among women than men.
Early signs and symptoms of Addison’s disease are like other common health disorders, like depression or influenza. The patient might experience:
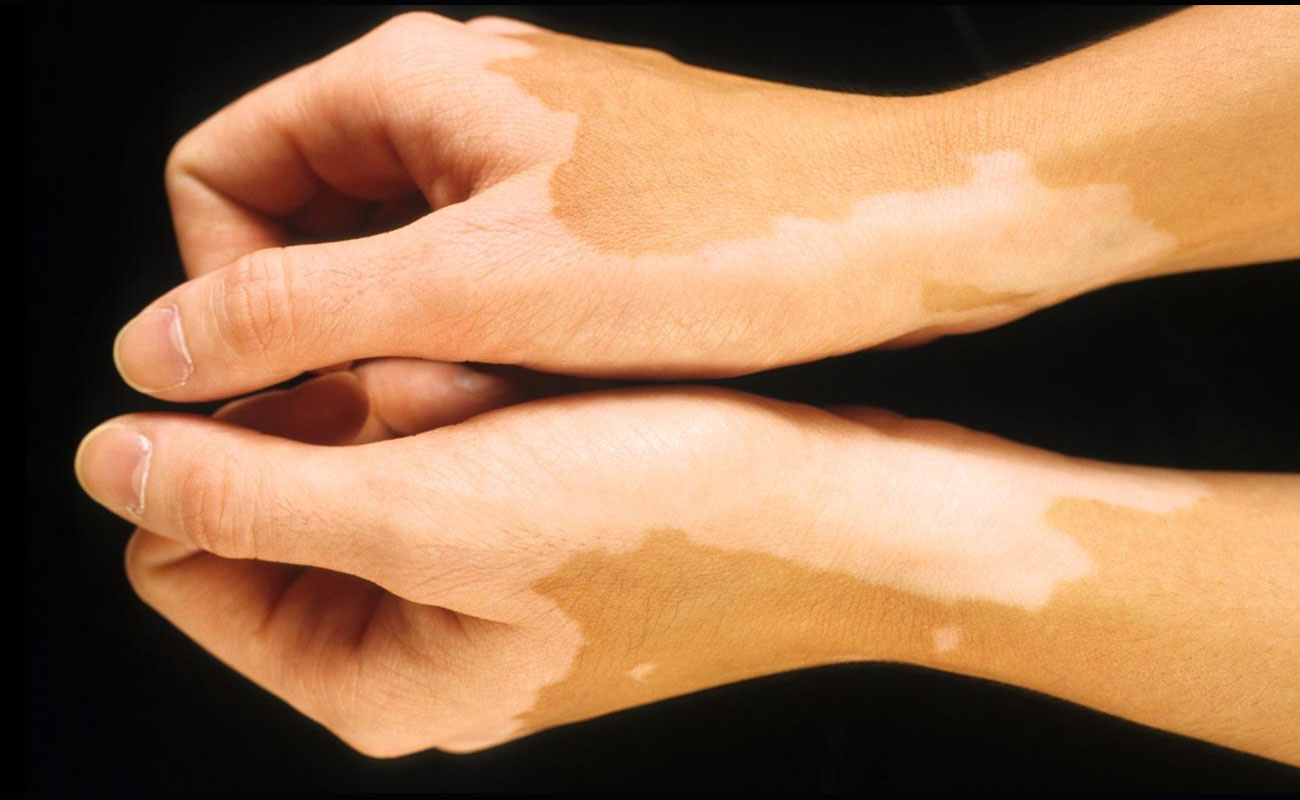
Over the course of time, the patient may experience these problems in a severe way or get involved in further symptoms, such as faintness, black out, cramps and fatigue (lack of energy and motivation). Also, small areas of darkened skin, or darkened lips or gums are rare but expected.
Although these symptoms are not always triggered by Addison’s disease, you’d better pay your doctor a visit for further investigation of the causes.
Usually the signs and symptoms of Addison's disease grow slowly (mostly, over a couple of months). Some of them are as follows:
Acute adrenal failure
The signs and symptoms of Addison's disease might sometimes appear abruptly. In these cases (mostly fall into the category of acute adrenal failure), the signs and symptoms might appear as follows:
The two main categorizations of Addison’s disease are: primary adrenal insufficiency and secondary adrenal insufficiency. The physician needs to identify the type of the Addison’s disease In order to treat the condition.
Primary adrenal Insufficiency happens when the adrenal glands are severely injured and as the result no hormones could be produced. This kind of Addison’s disease usually occurs when the immune system attacks the adrenal glands (an autoimmune disease). In an autoimmune disease, the body’s immune system confuses organs or areas of the body with viruses, bacteria, or some other outside invaders.
Some other causes of primary adrenal insufficiency may be as follows:
Secondary adrenal insufficiency happens when the pituitary gland in the brain is unable to produce adrenocorticotropic hormone (ACTH). ACTH instruct the adrenal gland for the time of releasing hormones.
If the patient does not follow his doctor’s prescription regarding corticosteroid, it is possible that he develops adrenal insufficiency. Corticosteroids helps control chronic health disorders such as asthma.
Diagnosing adrenal insufficiency in the primary stages is too difficult. The patient's medical records as well as the symptoms appearing on him, particularly the dark tanning of the skin, would be the lead indication of the disorder for the physician.
However, Addison's disease is diagnosed by laboratory tests. The primary goal of the laboratory tests is to determine whether cortisol levels are insufficient or not and then to find out what the causes are. Also, X-ray exams of the adrenal and pituitary glands are very useful in finding the cause.
ACTH Stimulation Test is the most precise test used for Addison's disease diagnoses. In this test, blood cortisol, urine cortisol, or sometimes both are measured before and after a synthetic form of ACTH is injected. In the rapid ACTH test, blood cortisol is repeatedly measured 30 to 60 minutes after an intravenous ACTH injection. Rise in levels of blood and urine cortisol is the normal response after an injection of ACTH. Those patient with any kind of adrenal insufficiency hardly respond or do not respond at all.
If the response to the short ACTH test is not normal, then for determining the cause of adrenal insufficiency, a "long" CRH stimulation test will be performed. In this test, intravenous synthetic CRH is injected and blood cortisol is measured before and 30, 60, 90, and 120 minutes after the injection. High ACTHs is indicated in those with primary adrenal insufficiency while there is no production of cortisol. On the other hand, deficient cortisol responses is observed in those patients with secondary adrenal insufficiency while there is no ACTH responses or they are delayed. Absent ACTH response points to the pituitary as the cause; a delayed ACTH response points to the hypothalamus as the cause.
In those patients suspected of having an Addison crisis, the medical practitioner has to instantly start the treatment with injections of fluids, salt, and glucocorticoid hormones. Although when the patient is being treated for the crisis a consistent diagnosis is not likely, diagnosing could be done through measuring blood ACTH and cortisol during the crisis and before giving glucocorticoids. When the crisis is controlled and medications have been stopped, the physician will delay further testing for up to 1 month in order to get an accurate diagnosis.
When a primary adrenal insufficiency is diagnosed, the x-ray exams of the stomach might be taken to know whether the adrenals show any signs of calcium deposits. Calcium deposits might be an indication of TB. Also, a tuberculin skin test could be used.
When the cause is secondary adrenal insufficiency, medical practitioner might use different imaging tools to find the size and shape of the pituitary gland. The most common tool to do so is the CT scan. It creates a sequence of x-ray pictures giving a cross-sectional image of an organ. The pituitary functioning and its ability to secrete the other hormones are tested as well.

If the adrenal glands don’t create essential hormones required by the body, the disorder is treated through replacing the hormones the person actually needs. Cortisol is substituted with a corticosteroid like dexamethasone, hydrocortisone, and prednisone. Considering which replacement is used, the corticosteroid is taken one to three times a day.
Aldosterone is substituted with a mineralocorticoid known as fludrocortisone acetate which might as well taken once or twice a day. Since those patients with secondary adrenal insufficiency typically have their adrenals still producing aldosterone, they do not need aldosterone replacement.
At the time of adrenal crisis, since the low levels of blood pressure, sodium, blood glucose, and high levels of potassium may put the patient in the great risk, immediate IV injections of steroids and IV saline solutions of sugars in the form of dextrose can be supplied in order to get quick improvement.
Those people with adrenal insufficiency must pay close attention to the times when stress on the body is increased. The time of surgery, severe injury or disease, and pregnancy period are some of the most important ones. Arduous sports or exercise or night shifts work may as well have some negative impacts on cortisol levels. Some of the mentioned kinds of stress would need some extra treatment to recover, such as “stress” dosages of corticosteroids, which could be taken both intravenously and orally. Once the stress situation is over for the patients, they could typically get back to their normal quantities of medications.
If patients with Addison’s disease are aldosterone deficient, a diet with high sodium could come in handy. The physicians could provide them with precise suggestions regarding the quantity of needed sodium.
Steroids treatment could have dangerous consequences such as osteoporosis (the condition which could result in bones fracture or less dense bones). Consumption of enough calcium and vitamin D may help prevent the condition and maintain good health of the bone.
Submit Comment