Acanthosis nigricans is a skin condition that causes one or more areas of skin to darken and thicken. The affected skin often feels velvety.
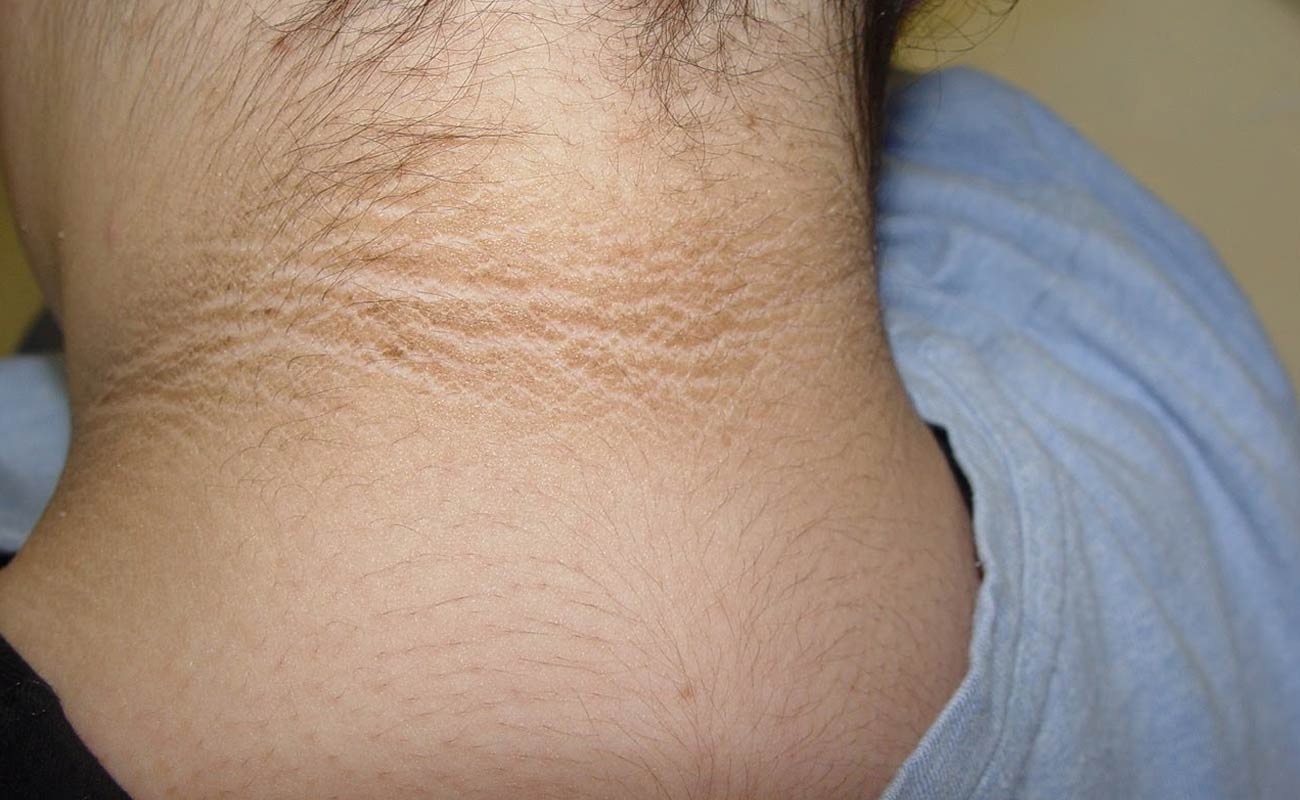
People who get this skin condition sometimes mistakenly believe that a dye or something else they touched has discolored their skin. Vigorous scrubbing will not get rid of the darkened skin.
Acanthosis nigricans is not contagious. It is not harmful. Sometimes, it is a warning sign of a health problem that requires medical attention. For this reason, it is important to see a dermatologist if you notice an area of darker, thicker skin.
If you notice a change to your skin, you should see a dermatologist. Small changes may seem like nothing. Sometimes a small change is an early warning sign. AN can be a sign of pre-diabetes, which increases your risk of getting diabetes. Making lifestyle changes before diabetes develops can prevent diabetes.
Some people get AN from a medicine that they are taking. Changing medicines might be an option for you. Other times, these dark patches have no connection to any medical condition. A dermatologist can help you find out what’s causing your skin changes.
If you have acanthosis nigricans, you'll have thickened, brownish-grey or black patches of skin.
The patches will be dry and rough, feeling similar to velvet. They may also be itchy.
These patches may occur anywhere, but are usually seen around the neck, in the armpit, around the groin and sometimes in other skin folds. Occasionally, the skin over the joints of the fingers and toes may be affected, as well as the lips, palms of the hands and soles of the feet.
The patches usually develop slowly over time. Patches that grow and spread quickly are more likely to be associated with cancer. In these cases, the mouth, tongue, throat, nose and windpipe may also be affected.
You may also have lots of tiny finger-like growths from the patches. This is known as papillomatosis.
There may also be skin tags around the affected area. These are small flesh-colored or pigmented growths that hang off the skin and look a bit like warts.
Acanthosis nigricans has been associated with:
Too Much Insulin
The most frequent trigger for acanthosis nigricans is too much insulin in your bloodstream.
When you eat, your body converts carbohydrates into sugar molecules such as glucose. Some of this glucose is used for energy in your cells while the rest is stored. The hormone insulin must allow glucose to enter cells so that the cells can use glucose for energy.
Overweight people tend to develop resistance to insulin over time. Although the pancreas is making insulin, the body can’t use it properly. This creates a buildup of glucose in the bloodstream, which can result in high levels of both blood glucose and insulin in your bloodstream.
Excess insulin causes normal skin cells to reproduce at a rapid rate. For those with dark skin, these new cells have more melanin. This increase in melanin produces a patch of skin that’s darker than the skin surrounding it. Thus, the presence of acanthosis nigricans is a strong predictor of future diabetes. If too much insulin is indeed the cause, it’s relatively easy to correct with proper diet, exercise, and blood sugar control.
Medications
Acanthosis nigricans can also be triggered by certain medications such as birth control pills, human growth hormones, thyroid medications, and even some bodybuilding supplements. All of these medications can cause changes in insulin levels. Medications used to ease the side effects of chemotherapy have also been linked to acanthosis nigricans. In most cases, the condition clears up when the medications are discontinued.
Other Potential Causes
In rare cases, acanthosis nigricans can be caused by:

Acanthosis nigricans is typically diagnosed clinically. A skin biopsy may be needed in unusual cases. If no clear cause is obvious, it may be necessary to search for one. Blood tests, an endoscopy, or X-rays may be required to eliminate the possibility of diabetes or cancer as the cause.
On biopsy, hyperkeratosis, epidermal folding, leukocyte infltration, and melanocyte proliferation may be seen.
Acanthosis nigricans should be distinguished from the casal collar appearing in pellagra.
In middle-aged and older patients with extensive skin or severe skin and mucosal findings, a workup for internal malignancy is indicated.
The vast majority of cases are due to obesity and/or insulin resistance. Screen for diabetes with a glycosylated hemoglobin level or glucose tolerance test.
Screen for insulin resistance; a good screening test for insulin resistance is a plasma insulin level, which will be high in those with insulin resistance. This is the most sensitive test to detect a metabolic abnormality of this kind because many younger patients do not yet have overt diabetes mellitus and an abnormal glycosylated hemoglobin level, but they do have a high plasma insulin level.
The primary aim of treatment is to correct the underlying disease process. Often correcting the underlying cause results in resolution of the lesions.
In hereditary acanthosis nigricans, lesions tend to enlarge gradually before stabilising and/or regressing on their own.
There is no specific treatment for acanthosis nigricans. Treatments considered are used primarily to improve cosmetic appearance and include topical retinoids, dermabrasion and laser therapy.
Final outcome of acanthosis nigricans varies depending on the cause of acanthosis nigricans. Benign conditions either on their own or through lifestyle changes and/or treatment have good outcomes. However, the prognosis for patients with malignant acanthosis nigricans is often poor. The associated cancer is often advanced and the average survival of these patients is approximately 2 years.
Most cases of acanthosis nigricans are harmless and not a sign of anything serious. The skin patches often fade with time as the underlying condition is treated.
If you have inherited acanthosis nigricans from your parents, your patches may gradually get bigger before staying the same or eventually fading on their own.
Only in cases where there is underlying cancer is the situation very serious. If the tumour is successfully treated, the condition may disappear, but unfortunately the types of cancer that cause acanthosis nigricans tend to spread quickly and a cure is often not possible.
Submit Comment