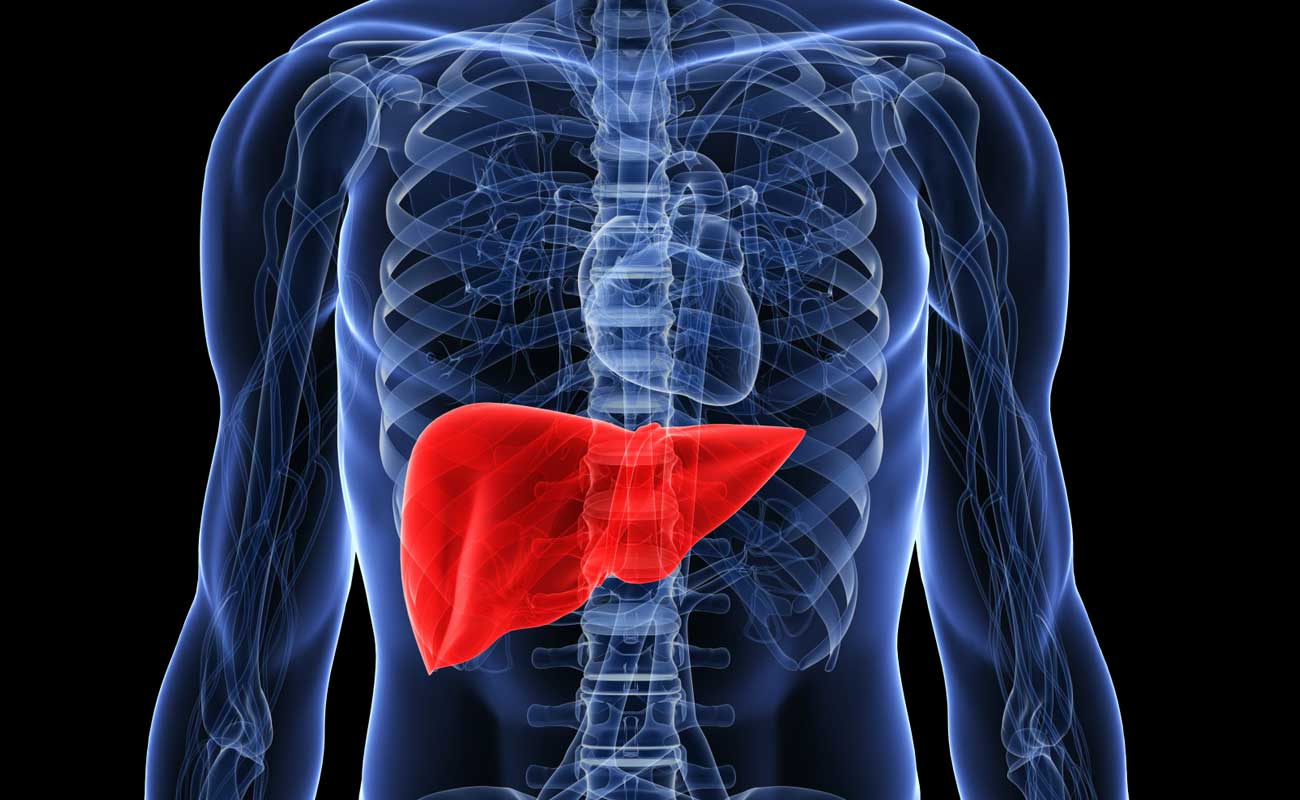
Liver disease related to alcohol consumption fits into 1 of 3 categories: fatty liver, alcoholic hepatitis, or cirrhosis. Fatty liver, which occurs after acute alcohol ingestion, is generally reversible with abstinence and is not believed to predispose to any chronic form of liver disease if abstinence or moderation is maintained. Alcoholic hepatitis is an acute form of alcohol-induced liver injury that occurs with the consumption of a large quantity of alcohol over a prolonged period of time; it encompasses a spectrum of severity ranging from asymptomatic derangement of biochemistries to fulminant liver failure and death. Cirrhosis involves replacement of the normal hepatic parenchyma with extensive thick bands of fibrous tissue and regenerative nodules, which results in the clinical manifestations of portal hypertension and liver failure.
Forms of Alcoholic Liver Disease | |||
Parameter | Fatty Liver | Alcoholic Hepatitis | Cirrhosis |
Histologic specificity | No | No | No |
Prognosis | Excellent | Variable | Guarded |
Reversible? | Yes | Variable | Generally no |
If you do experience early symptoms of ARLD, these are often quite vague, such as:
As the liver becomes more severely damaged, more obvious and serious symptoms can develop, such as:

Alcoholic liver disease occurs after years of heavy drinking. Over time, scarring and cirrhosis can occur. Cirrhosis is the final phase of alcoholic liver disease.
Alcoholic liver disease does not occur in all heavy drinkers. The chances of getting liver disease go up the longer you have been drinking and more alcohol you consume. You do not have to get drunk for the disease to happen.
The disease seems to be more common in some families. Women may be more likely to have this problem than men.
Alcohol-related liver disease (ARLD) is often first suspected when tests for other medical conditions show a damaged liver.

This is because the condition causes few obvious symptoms in the early stages.
If a doctor suspects ARLD, they'll usually arrange a blood test to check how well your liver is working. They may also ask about your alcohol consumption.
It's important to be totally honest about how much and how often you drink alcohol to avoid further unnecessary testing. This could lead to a delay in the treatment you need.
Blood tests used to assess the liver are known as liver function tests. However, liver function tests can be normal at many stages of liver disease.
Blood tests can also detect if you have low levels of certain substances, such as a protein called serum albumin, which is made by the liver. A low level of serum albumin suggests your liver isn't functioning properly.
A blood test may also look for signs of abnormal blood clotting, which can indicate significant liver damage.
Lab Tests Online has more information on liver function tests.
If your symptoms or liver function test suggest an advanced form of ARLD – either alcoholic hepatitis or cirrhosis – you may need further tests. These are described below.
Scans may be needed to produce detailed images of your liver. This may include:
Some scans may also measure the stiffness of the liver, which is a good indication of whether your liver is scarred.
During a liver biopsy, a fine needle is inserted into your body (usually between your ribs). A small sample of liver cells is taken and sent to a laboratory to be examined under a microscope.
The biopsy is usually carried out under local anaesthetic, either as a day case or with an overnight stay in hospital.
Specialist doctors will examine the liver biopsy tissue under the microscope to determine the degree of scarring in the liver and the cause of the damage.
An endoscope is a long, thin, flexible tube with a light and a video camera at one end. During an endoscopy, the instrument is passed down your oesophagus (the long tube that carries food from the throat to the stomach) and into your stomach.
Pictures of your oesophagus and stomach are transmitted to an external screen. The doctor will be looking for swollen veins (varices), which are a sign of cirrhosis.
ARLD treatment has two goals. The first is to help you stop drinking. This can prevent further liver damage and encourage healing. The second is to improve your liver health.
If you have ARLD, your doctor may recommend:
It’s important to note that taking vitamin A and alcohol together can be deadly. Only people who have stopped drinking can take these supplements. Supplements will not cure liver disease, but they can prevent complications like malnutrition.

In general, the more you drink above the safe limits, the more harmful alcohol is likely to be.
And remember, binge drinking can be harmful even though the weekly total may not seem too high. For example, if you only drink alcohol once or twice a week but when you do you drink 4-5 pints of beer each time, or a bottle of wine each time, this is a risk to your health.
One unit of alcohol is 10 ml (1 cl) by volume, or 8 g by weight, of pure alcohol. For example:
But remember, many wines and beers are stronger than the more traditional ordinary strengths. A more accurate way of calculating units is as follows. The percentage alcohol by volume (% abv) of a drink equals the number of units in one litre of that drink. For example:
Submit Comment