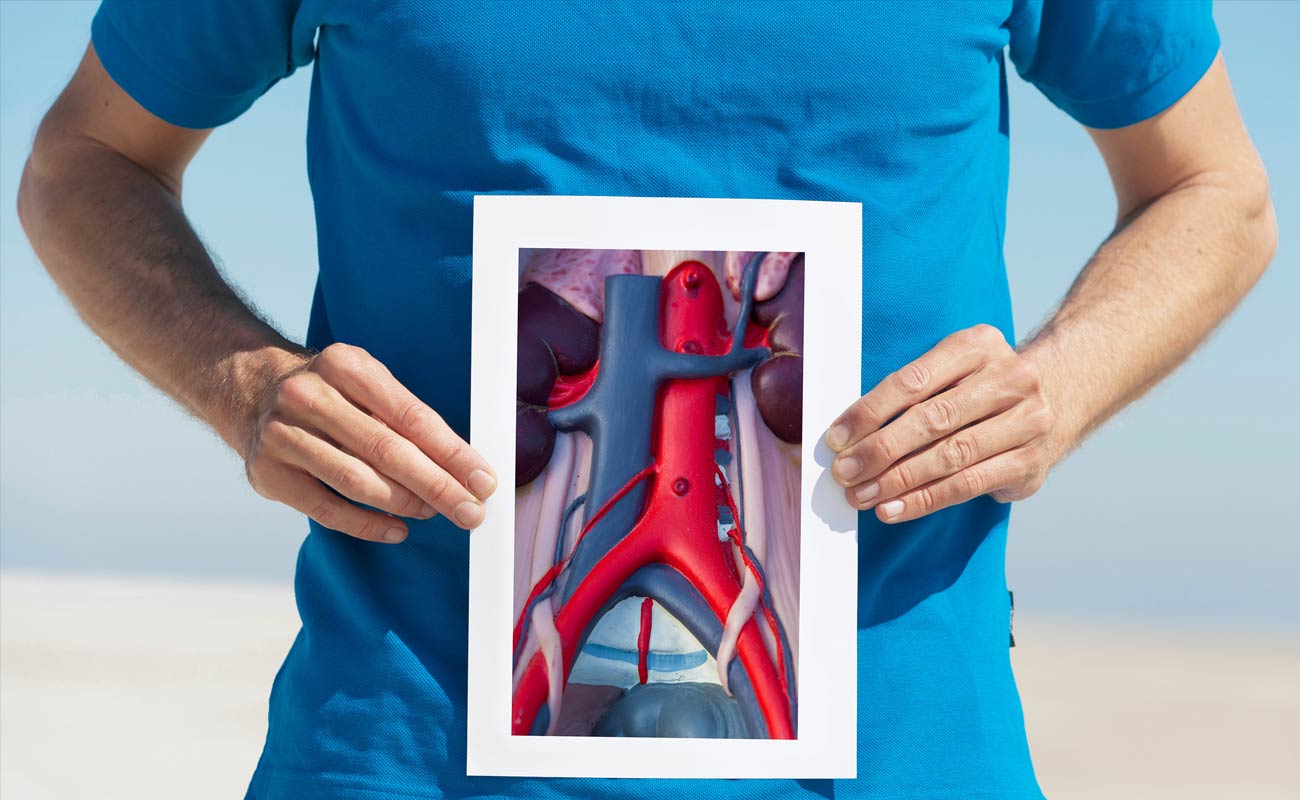
An abdominal aortic aneurysm (AAA) is a swelling (aneurysm) of the aorta – the main blood vessel that leads away from the heart, down through the abdomen to the rest of the body.
The abdominal aorta is the largest blood vessel in the body and is usually around 2cm wide – roughly the width of a garden hose. However, it can swell to over 5.5cm – what doctors class as a large AAA.
Large aneurysms are rare, but can be very serious. If a large aneurysm bursts, it causes huge internal bleeding and is usually fatal.
The bulging occurs when the wall of the aorta weakens. Although what causes this weakness is unclear, smoking and high blood pressure are thought to increase the risk of an aneurysm.
AAAs are most common in men aged over 65. A rupture accounts for more than 1 in 50 of all deaths in this group and a total of 6,000 deaths in England and Wales each year.
This is why all men are invited for a screening test when they turn 65. The test involves a simple ultrasound scan, which takes around 10-15 minutes.
Abdominal aortic aneurysms often grow slowly and usually without symptoms, making them difficult to detect. Some aneurysms will never rupture. Many start small and stay small, although many expand over time. Others expand quickly. Predicting how fast an abdominal aortic aneurysm may enlarge is difficult.
As an abdominal aortic aneurysm enlarges, some people may notice:
If you have any of these signs and symptoms, such as sudden severe back or abdominal pain, get immediate emergency help.
When to see a doctor
You should see your doctor if you have any of the symptoms listed above. The recommendations below are for those who have no symptoms.
Because being male and smoking significantly increase the risk of abdominal aortic aneurysm, men ages 65 to 75 who have ever smoked cigarettes should have a screening for abdominal aortic aneurysms using abdominal ultrasound. If you are a man between ages 65 and 75 and you have never smoked, your doctor will decide on the need for an abdominal ultrasound, usually based on other risk factors, such as a family history of aneurysm. Those with a family history of aneurysm may have an ultrasound at age 60.
There isn't enough evidence to determine whether women ages 65 to 75 who have ever smoked cigarettes or have a family history of abdominal aortic aneurysm would benefit from abdominal aortic aneurysm screening. Ask your doctor if you need to have an ultrasound screening based on your risk factors. Women who have never smoked generally don't need to be screened for the condition.
AAAs that haven’t ruptured are most often diagnosed when a doctor is scanning or examining your abdomen for another reason.
If your doctor suspects that you may have one, they will feel your stomach to see if it’s rigid or contains a pulsing mass. They may also check the blood flow in your legs or use one of the following tests:
The best way to prevent getting an aneurysm, or reduce the risk of an aneurysm growing bigger and possibly rupturing, is to avoid anything that could damage your blood vessels.
This includes:
If your GP finds out you have high blood pressure or a high cholesterol level, you may be prescribed medication for both. This will reduce the risk of developing an abdominal aortic aneurysm (AAA).
Smoking is a major risk factor for aneurysms because it causes atherosclerosis (hardening of the arteries) and raises your blood pressure.
Tobacco smoke contains substances that can damage the walls of the arteries.
It is known that smokers are seven times more likely than non-smokers to develop an AAA.
The more you smoke, the greater your risk. People who regularly smoke more than 20 cigarettes a day may have more than 10 times the risk of non-smokers.
Eating a high-fat diet increases your risk of atherosclerosis.
It’s especially important to limit the amount of foods you eat that are high in saturated fat, such as biscuits, cakes, butter, sausages and bacon.
This is because eating too much saturated fat can lead to high cholesterol, which can build up in the artery walls.
Being active and doing regular exercise lowers blood pressure by keeping your heart and blood vessels in good condition.
Regular exercise can also help you lose weight, which will also help lower your blood pressure.
Adults should do at least 150 minutes (two hours and 30 minutes) of moderate-intensity aerobic activity every week.
Examples of moderate intensity activity include cycling or fast walking.
For it to count, the activity should make you feel warm and slightly out of breath. Someone who is overweight may only have to walk up a slope to get this feeling.
Physical activity can include anything from sport to walking and gardening.
Being overweight forces your heart to work harder to pump blood around your body. This can raise your blood pressure, which in turn puts pressure on your arteries.
If you need to shed some weight, it's worth remembering that losing just a few pounds will make a big difference to your blood pressure and overall health.

Treatment depends on the size of the aneurysm.
Small AAAs (less than 5 cm in diameter)
Have a very low risk of rupturing, but should be watched.
Larger (more than 5.0-5.5 cm in diameter)
Rapidly enlarging and AAAs causing symptoms are usually repaired.
Open surgery requires placement of a prosthetic graft.
Endovascular aneurysm repair (EVAR) is a less invasive treatment.
Submit Comment